Polycystic Ovary Syndrome (PCOS) represents one of the most prevalent endocrine disorders affecting women of reproductive age, characterized by a complex interplay of hormonal imbalances that frequently manifest as persistent, treatment-resistant acne. Unlike the transient breakouts associated with the typical menstrual cycle, PCOS-related acne is driven by systemic androgen excess, necessitating a multi-faceted therapeutic approach that goes beyond standard over-the-counter topical treatments. Medical experts and dermatologists emphasize that understanding the underlying physiological drivers—specifically the roles of the pituitary gland, insulin sensitivity, and androgen receptors—is essential for patients seeking long-term dermatological relief and endocrine stability.

The Endocrine Foundation of PCOS-Induced Skin Pathology
The pathogenesis of acne in the context of PCOS begins with a disruption of the Hypothalamic-Pituitary-Ovarian (HPO) axis. Under normal physiological conditions, the pituitary gland serves as the control center, regulating the production of estrogen, progesterone, and androgens. In a healthy cycle, these hormones fluctuate in a choreographed sequence to facilitate ovulation and maintain skin health. However, in patients with PCOS, the signaling process is frequently compromised. The pituitary gland may produce elevated levels of luteinizing hormone (LH), which stimulates the theca cells in the ovaries to produce an excess of androgens, primarily testosterone.
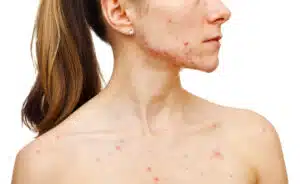
While androgens are necessary for bone density and reproductive tissue repair in women, an overabundance leads to the overstimulation of sebaceous glands. These glands, located within the skin’s pores, begin to produce excessive sebum (oil). When this oil mixes with dead skin cells, it creates an anaerobic environment ripe for the proliferation of Cutibacterium acnes, the bacteria responsible for inflammatory lesions. Clinical data suggests that PCOS-related acne is often "hormonal" in distribution, typically appearing along the jawline, chin, and neck, and is characterized by deep, painful cystic nodules rather than simple surface comedones.
The Insulin-Androgen Connection and Dietary Influence
A critical but often overlooked component of PCOS is insulin resistance. Statistics indicate that a significant percentage of women with PCOS—both lean and those with higher BMIs—exhibit some degree of insulin resistance. When the body’s cells become less responsive to insulin, the pancreas compensates by secreting higher levels of the hormone. This hyperinsulinemia acts as a co-gonadotropin, further prompting the ovaries to secrete testosterone and decreasing the production of Sex Hormone-Binding Globulin (SHBG). SHBG is a protein that normally binds to testosterone in the blood, rendering it inactive; when SHBG levels drop, more "free" testosterone is available to aggravate the skin.
This biological mechanism provides the scientific basis for dietary interventions. Many clinical practitioners recommend a low-glycemic index (GI) diet to stabilize insulin levels. Furthermore, observational studies and patient reports have frequently linked dairy consumption to exacerbated acne. The hypothesis posits that dairy contains growth hormones and can increase levels of Insulin-like Growth Factor 1 (IGF-1), which mimics the effects of insulin on the sebaceous glands. For many patients, the elimination of dairy can result in noticeable skin clearance within a matter of weeks, as it removes an external trigger for insulin and androgen spikes.

Pharmacological Interventions: Prescription Retinoids
When lifestyle and dietary changes are insufficient, dermatologists often turn to retinoids, a class of medications derived from Vitamin A. Since their introduction to the dermatological market in 1971, retinoids have become a cornerstone of acne therapy. They function by accelerating cell turnover and preventing the hyperkeratinization of the follicles—essentially ensuring that dead skin cells do not clog pores.
For moderate to severe PCOS acne, over-the-counter retinol is rarely potent enough. Prescription-strength topical retinoids, such as Tretinoin (Retin-A) or Adapalene, are frequently required. In the most recalcitrant cases, oral Isotretinoin (commonly known by the former brand name Accutane) may be prescribed. Isotretinoin is unique in that it addresses all four major causes of acne: excess oil production, clogged pores, bacterial growth, and inflammation. However, the use of oral retinoids in women of childbearing age is strictly regulated due to the high risk of severe birth defects. Patients are typically required to participate in monitoring programs, such as iPLEDGE in the United States, which mandate the use of two forms of contraception and regular pregnancy testing.
Antiandrogen Therapy: Targeting the Root Cause
Because PCOS acne is fundamentally a result of "male" hormones acting on female skin, antiandrogen medications offer a targeted solution. These drugs, known as androgen antagonists, work by blocking androgen receptors or inhibiting the production of androgens.
- Spironolactone: Originally developed as a potassium-sparing diuretic for hypertension, Spironolactone is widely used "off-label" by dermatologists to treat hormonal acne. It competes with androgens for receptor sites in the sebaceous glands, effectively "shielding" the skin from the effects of testosterone. Clinical trials have shown significant reductions in inflammatory lesions in women with PCOS when using Spironolactone over a period of three to six months.
- Cyproterone Acetate: Frequently used in Europe and Canada, often in combination with estrogen, this potent antiandrogen reduces the production of sebum and lowers serum testosterone levels.
- Flutamide: While effective, Flutamide is less commonly used for acne due to concerns regarding potential liver toxicity, making Spironolactone the preferred choice for most clinicians.
The Role of Combined Oral Contraceptives
For many years, combined oral contraceptives (COCs) have been the first-line treatment for managing the systemic symptoms of PCOS, including irregular cycles and hirsutism. COCs contain synthetic versions of estrogen and progestin. These hormones work in tandem to suppress the pituitary gland’s production of LH and FSH, thereby reducing ovarian androgen production. Additionally, the estrogen component in birth control pills stimulates the liver to produce more SHBG, further lowering free testosterone levels.

The FDA has approved several specific formulations for the treatment of acne, including those containing norgestimate, norethindrone, or drospirenone (such as Yaz or Ortho Tri-Cyclen). However, the medical community maintains a cautious approach for certain populations. Women with PCOS who are obese, smokers over the age of 35, or those with a history of migraines with aura are at an increased risk for venous thromboembolism (blood clots). For these patients, the risks of hormonal birth control may outweigh the dermatological benefits, necessitating alternative therapies.
Chronology of Treatment and Managing Expectations
Patients embarking on a PCOS acne treatment plan must be prepared for a slow timeline. Unlike bacterial infections that may respond to antibiotics within days, hormonal shifts take time to manifest on the skin’s surface. A typical timeline for treatment efficacy includes:

- Weeks 1–4: Potential "purging" period where skin may appear worse as deep-seated clogs are pushed to the surface.
- Month 2: Stabilization of oil production.
- Months 3–6: Significant reduction in new cystic lesions and beginning of the healing process for post-inflammatory hyperpigmentation (scarring).
Psychosocial Impact and the Vicious Cycle of Stress
The psychological burden of PCOS acne cannot be overstated. Studies published in the Indian Dermatology Online Journal and other clinical publications highlight that women with PCOS suffer from higher rates of anxiety, depression, and social withdrawal due to their physical symptoms. This creates a physiological "vicious cycle": the stress of having acne triggers the adrenal glands to produce cortisol and additional androgens, which in turn causes more acne.
Stress management techniques, including mindfulness-based stress reduction (MBSR), yoga, and cognitive-behavioral therapy, are increasingly recognized as valid adjunct treatments. By lowering the body’s systemic stress response, patients can reduce the "adrenal" contribution to their androgen levels, supporting the efficacy of their primary medical treatments.

Broader Implications and Integrated Care
The management of PCOS hormonal acne is more than a cosmetic endeavor; it is a vital part of managing a systemic metabolic condition. Persistent acne in adulthood often serves as a clinical marker for underlying insulin resistance or lipid imbalances that, if left unaddressed, could lead to Type 2 diabetes or cardiovascular disease later in life.
A journalistic analysis of current medical trends suggests a move toward "Integrated Care Models." Rather than seeing a dermatologist in isolation, the most successful outcomes for PCOS patients occur when dermatologists, endocrinologists, and registered dietitians collaborate. This holistic approach ensures that while the skin is being treated with retinoids or antiandrogens, the underlying metabolic drivers are being managed through diet and lifestyle, providing a sustainable path to both clear skin and overall endocrine health. In summary, while PCOS presents a significant challenge to skin health, the combination of modern pharmacology, targeted nutritional strategies, and stress management offers a robust framework for patients to regain control over their appearance and their wellbeing.