Marking World TB Day 2026, the World Health Organization (WHO) has issued a high-level call to action for the international community to accelerate efforts toward the eradication of tuberculosis (TB). Under the evocative theme, “Yes! We can end TB: Led by countries, powered by people,” the organization is championing a paradigm shift in how the disease is detected and treated. Central to this new strategy is the deployment of groundbreaking innovations, including point-of-care diagnostic tests and non-invasive tongue swabs, which are designed to reach vulnerable populations more effectively than traditional methods. These advancements arrive at a critical juncture as the global health community struggles to maintain progress in the face of dwindling funding and the persistent shadow of antimicrobial resistance.
A New Era of Decentralized Diagnostics
The cornerstone of the WHO’s latest guidance is the introduction of portable, simple-to-use diagnostic tools that can be operated near the point-of-care. Historically, TB diagnosis has relied heavily on centralized laboratories, necessitating the transport of samples over long distances, which often resulted in significant delays or lost results. The new molecular diagnostics recommended by the WHO are designed to bypass these logistical hurdles. These devices can operate on battery power and deliver highly accurate results in less than one hour. Furthermore, they are available at less than half the cost of many existing molecular platforms, making them a viable option for low- and middle-income countries.
Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, emphasized the potential of these tools to reshape the public health landscape. He noted that bringing fast, accurate diagnosis closer to the community is essential for saving lives and curbing the transmission of the bacteria. By identifying cases earlier, health systems can initiate treatment regimens before the disease spreads further within households and communities. Beyond their application for TB, these versatile devices can be adapted to test for other infectious diseases, such as HIV, mpox, and human papillomavirus (HPV), facilitating a "one-stop-shop" model for integrated health services.
Revolutionary Sample Collection: The Shift to Tongue Swabs
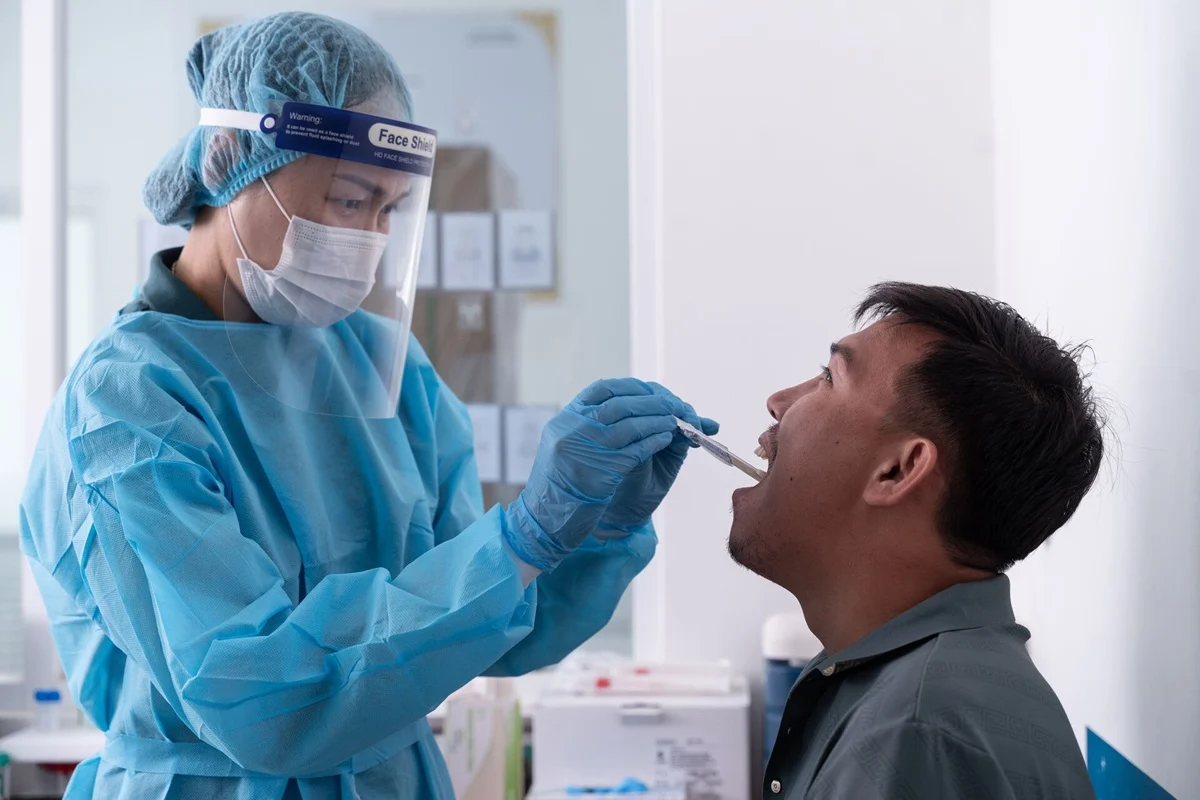
One of the most significant barriers to TB testing has been the reliance on sputum—a thick mucus coughed up from the lower airways. Many patients, particularly children, adolescents, and people living with HIV, struggle to produce an adequate sputum sample, leading to underdiagnosis and increased mortality. To address this, the WHO’s new guidelines recommend the use of tongue swabs as an alternative collection method. This non-invasive technique allows for easier sampling in a wider range of clinical and community settings, ensuring that those at the highest risk of dying from the disease are no longer overlooked by diagnostic protocols.
In addition to tongue swabs, the WHO is promoting a sputum pooling strategy to maximize efficiency in resource-constrained environments. By combining samples from multiple individuals and testing them in a single run, TB programs can significantly reduce the consumption of expensive reagents and decrease machine processing time. If a pool tests positive, individual samples are then tested to identify the infected person. This approach is specifically recommended for areas where diagnostic resources are exceptionally limited, allowing for broader surveillance without a proportional increase in costs.
The Global Burden and the Cost of Inaction
Tuberculosis remains one of the world’s most formidable infectious killers, despite being both preventable and curable. Current data indicates that more than 3,300 people succumb to the disease every day, and over 29,000 individuals fall ill. While global efforts have saved an estimated 83 million lives since the turn of the millennium, the momentum is currently at risk. The WHO warns that cuts in global health funding are threatening to reverse decades of gains. The uptake of rapid diagnostic tools has been historically slow due to high initial investment costs and a systemic reliance on centralized infrastructure.
The economic argument for investing in TB eradication is, however, overwhelming. According to Dr. Tereza Kasaeva, Director of the WHO’s Department for HIV, Tuberculosis, Hepatitis and Sexually Transmitted Infections, every dollar invested in TB prevention and care generates up to US$ 43 in health and economic returns. This high return on investment (ROI) stems from restored productivity, reduced healthcare costs, and the prevention of premature death among the most economically active segments of the population. Dr. Kasaeva argues that investing in TB is not merely a humanitarian gesture but a strategic political and economic choice for national governments.
Chronology of the Fight Against TB: From Discovery to 2026
The fight against tuberculosis has a long and complex history. It was on March 24, 1882, that Dr. Robert Koch announced his discovery of Mycobacterium tuberculosis, the bacterium that causes the disease. At that time, TB killed one out of every seven people living in the United States and Europe. World TB Day is observed annually on this date to commemorate Koch’s breakthrough and raise awareness about the ongoing epidemic.
In the early 2000s, the "DOTS" (Directly Observed Treatment, Short-course) strategy became the international standard, significantly improving cure rates. By 2014, the World Health Assembly adopted the "End TB Strategy," which aimed for a 90% reduction in TB deaths and an 80% reduction in the TB incidence rate by 2030. The 2023 United Nations High-Level Meeting on TB further solidified these commitments, with world leaders pledging to provide TB treatment to 45 million people between 2023 and 2027. The 2026 milestones are viewed as a critical checkpoint to determine if the world is on track to meet the 2030 Sustainable Development Goals.
Addressing the Research and Development Gap
Despite the promise of new diagnostic tools, the WHO underscores that ending the epidemic will require a massive surge in research and development (R&D). Global funding for TB research is currently estimated to be far below the US$ 5 billion annual requirement. This funding gap has stifled the development of new medicines, shorter treatment regimens, and, most importantly, an effective vaccine.
The current BCG (Bacille Calmette-Guérin) vaccine, which is over a century old, provides some protection against severe forms of TB in children but is largely ineffective in preventing pulmonary TB in adolescents and adults, who are the primary drivers of transmission. To bridge this gap, the WHO has launched the TB Vaccine Accelerator Council. This initiative aims to align governments, philanthropic funders, and the private sector to fast-track the development of next-generation vaccines. By coordinating investment and streamlining regulatory pathways, the Council hopes to ensure that once a viable vaccine is found, it is accessible equitably across the globe.
Implications for Health Security and Universal Coverage
The push to end TB is inextricably linked to the broader goals of health security and Universal Health Coverage (UHC). Tuberculosis often thrives in the gaps of a health system, affecting those who lack access to primary care or who live in overcrowded, impoverished conditions. By integrating TB services into the general health infrastructure and utilizing point-of-care diagnostics, countries can strengthen their overall capacity to respond to infectious threats.
Public health analysts suggest that the "one-stop-shop" diagnostic model could be a blueprint for future pandemic preparedness. The ability to pivot a diagnostic platform from TB to a novel pathogen in a matter of weeks would provide a level of agility that was sorely lacking during the early stages of the COVID-19 pandemic. Furthermore, by reducing the diagnostic delay for TB, health systems can mitigate the rise of multi-drug-resistant TB (MDR-TB), which remains a significant threat to global health security.
A Call for Decisive Leadership
As countries observe World TB Day 2026, the WHO’s message is clear: the tools to end TB exist, but the political will and financial backing must match the scale of the challenge. The organization is calling on governments to prioritize TB as a central pillar of their national health agendas. This includes not only the adoption of the latest WHO recommendations but also the protection of health budgets from austerity measures.
The success of the "Yes! We can end TB" campaign depends on a multi-sectoral approach that involves civil society, the private sector, and affected communities. By empowering people with the knowledge and tools to seek care, and by ensuring that the care they receive is fast, accurate, and affordable, the global community can finally close the chapter on one of history’s deadliest diseases. The innovations highlighted in 2026 represent more than just technological progress; they represent a renewed promise to the millions of people who continue to suffer from a disease that should have been eradicated long ago.