The World Health Organization (WHO) has issued a high-level call to action on World TB Day 2026, urging nations to drastically accelerate their efforts to eliminate tuberculosis (TB) through the rapid adoption of cutting-edge diagnostic innovations and expanded access to essential healthcare services. This year’s observance, held under the theme “Yes! We can end TB: Led by countries, powered by people,” highlights a pivotal moment in the global fight against one of history’s most persistent and deadly infectious diseases. With the release of new clinical guidelines focusing on point-of-care testing and non-invasive sampling methods, the WHO aims to bridge the diagnostic gap that currently leaves millions of cases undetected each year.
Tuberculosis remains a premier global health threat, claiming more than 3,300 lives every day despite being both preventable and curable. The WHO’s latest strategic push emphasizes the deployment of portable diagnostic tests and tongue-swab sampling, tools designed to move the frontline of detection from centralized, often inaccessible laboratories directly to the communities where patients live and work. By prioritizing these "near-point-of-care" solutions, the organization hopes to reverse a trend of stagnating progress caused by funding shortfalls and the lingering impacts of global health disruptions.
The Revolution in Diagnostic Accessibility
At the heart of the WHO’s 2026 recommendations is a suite of new diagnostic tools that promise to transform the landscape of TB detection. For decades, the gold standard for TB diagnosis has relied on sputum samples—thick phlegm coughed up from the lungs—and complex laboratory equipment that requires stable electricity and highly trained personnel. These requirements have historically excluded millions of people in rural or resource-poor settings from receiving a timely diagnosis.
The new guidelines introduce portable, battery-powered molecular tests that can deliver highly accurate results in less than an hour. These devices are not only simple to operate but are also available at less than half the cost of many existing molecular diagnostic platforms. By reducing the financial and logistical barriers to entry, the WHO expects countries to scale up testing at the primary healthcare level. This shift allows patients to receive a diagnosis and begin life-saving treatment during a single clinic visit, drastically reducing the "loss to follow-up" that occurs when patients must wait days or weeks for results from a distant lab.
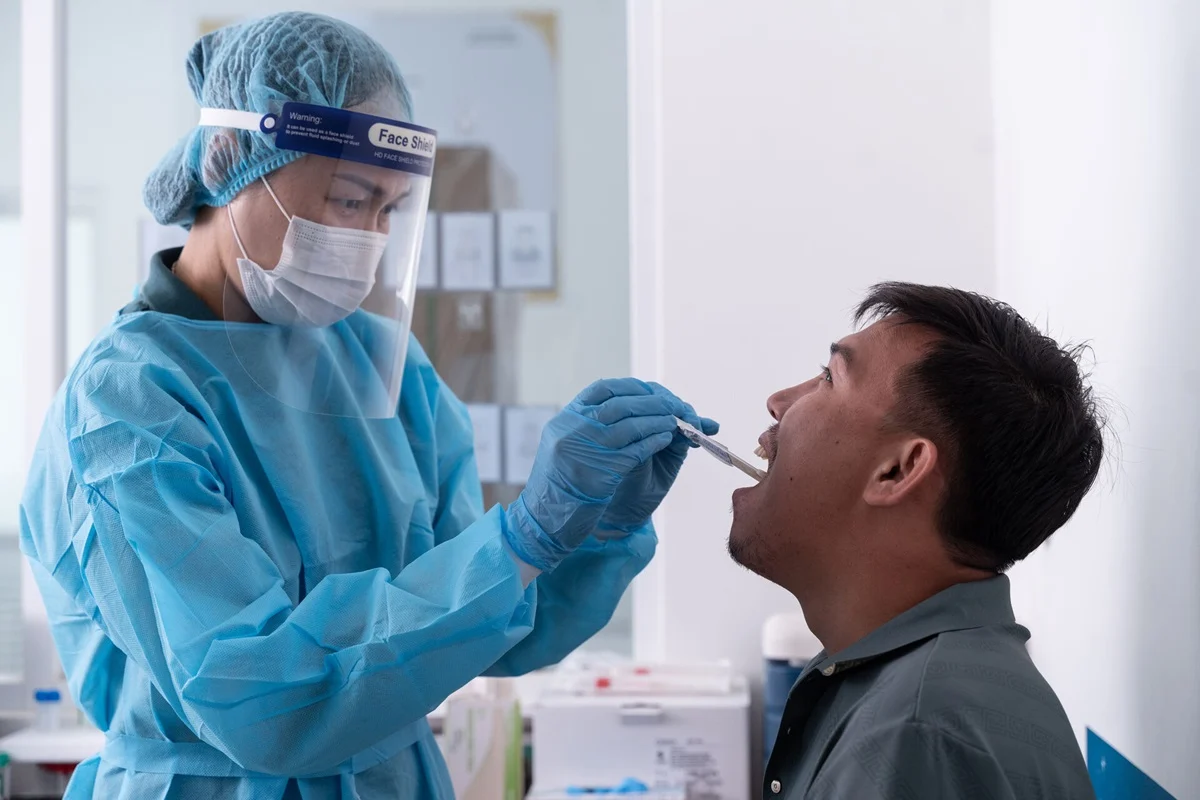
Furthermore, the introduction of tongue-swab testing represents a significant breakthrough for patient comfort and inclusivity. Many individuals, particularly children, adolescents, and people living with HIV, struggle to produce the sputum required for traditional tests. Tongue swabs provide a non-invasive alternative that can be collected easily by health workers or even the patients themselves. This innovation is expected to significantly increase detection rates among vulnerable populations who are at the highest risk of mortality from undiagnosed TB.
Economic and Societal Implications of TB Investment
The push for expanded TB services is not merely a clinical necessity but a strategic economic imperative. According to data released by the WHO Department for HIV, Tuberculosis, Hepatitis, and Sexually Transmitted Infections, every dollar invested in the fight against TB generates up to $43 in health and economic returns. This high return on investment (ROI) stems from restored productivity, reduced secondary transmission, and the prevention of catastrophic health expenditures for families.
Dr. Tereza Kasaeva, Director of the WHO TB department, emphasized that investing in TB elimination is a "strategic political choice." When TB remains unchecked, it drains national economies by disproportionately affecting the working-age population. Conversely, rapid implementation of WHO recommendations can stabilize communities and bolster national health security. The $43 ROI figure underscores that the cost of inaction far outweighs the cost of implementing these new diagnostic and treatment protocols.
A Chronology of Global TB Efforts
The fight against tuberculosis has seen various phases of momentum over the last quarter-century. Understanding the current 2026 mandate requires a look at the timeline of global interventions:
- 2000–2015: The Millennium Development Goals (MDGs) era saw the first major global push to halt and reverse the TB epidemic. During this period, an estimated 43 million lives were saved through improved DOTS (Directly Observed Treatment, Short-course) strategies.
- 2015: The United Nations adopted the Sustainable Development Goals (SDGs), which included a target to end the TB epidemic by 2030. This was supported by the WHO’s "End TB Strategy."
- 2018: The first-ever UN High-Level Meeting on TB took place, where world leaders committed to reaching 40 million people with care and 30 million with preventive treatment by 2022.
- 2020–2022: The COVID-19 pandemic severely disrupted TB services, leading to the first increase in TB deaths in over a decade as resources were diverted and lockdowns prevented patients from seeking care.
- 2023: A second UN High-Level Meeting reaffirmed global commitments, setting more ambitious targets for 2027, including reaching 90% of people with TB prevention and care services.
- 2026: The current milestone marks a critical "four-year-to-go" warning for the 2030 SDG targets. The focus has shifted from mere commitment to the "rapid implementation" of specific technological innovations like tongue swabs and battery-operated molecular tests.
Integrating Diagnostics: The One-Stop-Shop Model
One of the most promising aspects of the new diagnostic hardware is its versatility. The WHO has noted that the same platforms used for near-point-of-care TB testing can often be adapted to detect other high-priority pathogens, including HIV, mpox, and human papillomavirus (HPV). This multi-disease capability supports a "one-stop-shop" service model, which is central to the concept of universal health coverage.
By integrating TB testing with other essential health services, clinics can provide more patient-centered and equitable care. For instance, a person seeking an HIV viral load test could simultaneously be screened for TB, which remains the leading cause of death among people living with HIV. This integrated approach maximizes the utility of expensive equipment and reduces the burden on patients who would otherwise have to make multiple trips for different health concerns.
Addressing the Funding Gap and Research Deficit
Despite the clear economic benefits and the availability of new tools, the global TB response faces a daunting financial hurdle. Global funding for TB research currently hovers around $1 billion annually, which is significantly lower than the $5 billion estimated yearly requirement. This funding gap slows the development of new medicines, shorter treatment regimens, and, most importantly, an effective new TB vaccine.
The WHO’S TB Vaccine Accelerator Council, launched recently, is a cornerstone of the effort to bridge this gap. The Council aims to align governments, philanthropic organizations, and the private sector to fast-track the development of vaccines that could provide long-term protection for all age groups. Currently, the BCG vaccine—developed over a century ago—remains the only widely available vaccine, but its effectiveness in adults is limited. A modern vaccine is widely considered the "missing piece" required to truly end the epidemic.
In addition to research funding, there is a dire need for operational funding. Many low- and middle-income countries rely on international aid for their TB programs. However, recent shifts in global health priorities and economic pressures have threatened to reverse the gains made over the past two decades. The WHO is calling for domestic and international funders to treat TB as a central pillar of health security.
Innovative Strategies: Sputum Pooling
To maximize efficiency in resource-constrained settings, the 2026 guidelines also formally recommend "sputum pooling." This strategy involves combining samples from several individuals and testing them as a single batch. If the pool tests negative, all individuals in the group are cleared. If the pool tests positive, the individual samples are then tested separately to identify the infected person.
This method can significantly reduce the cost of reagents and the time machines spend running tests. During periods of high demand or when diagnostic commodities are in short supply, pooling allows TB programs to screen larger populations—such as those in prisons, refugee camps, or high-burden urban areas—much more quickly than individual testing would allow.
Global Progress and the Road to 2030
The 2026 World TB Day serves as a sobering reminder of the scale of the challenge. While global efforts have saved an estimated 83 million lives since the turn of the millennium, the fact that 29,000 people still fall ill with TB every day indicates that the current pace of progress is insufficient to meet the 2030 goal of ending the epidemic.
The WHO’s Director-General, Dr. Tedros Adhanom Ghebreyesus, has been vocal about the need for "decisive leadership." He noted that while the new tools are transformative, they are only effective if they reach the people who need them most. The disparity in access between high-income and low-income regions remains a primary obstacle. Scaling up urine-based tests for people with HIV and ensuring that rural clinics have the infrastructure to support battery-powered molecular diagnostics are essential steps in closing the diagnostic gap.
As the international community moves toward the 2027 deadline for the targets set at the 2023 UN High-Level Meeting, the focus remains on accountability. The WHO is urging countries to not only adopt the new guidelines but to also provide the political and financial backing necessary to implement them at scale. The 2026 theme, "Led by countries, powered by people," reflects a shift toward local ownership of the TB response, empowering communities to take the lead in identifying cases and supporting patients through the duration of their treatment.
In conclusion, the 2026 World TB Day marks a technological and strategic pivot. The introduction of tongue swabs, sputum pooling, and portable molecular diagnostics offers a roadmap to overcome the logistical barriers that have long protected the TB bacterium. However, without a significant increase in global funding and a commitment to equitable access, these innovations may remain out of reach for the millions of people who continue to suffer from this ancient but curable disease. The WHO’s call is clear: the tools to end TB exist; what remains is the global will to deploy them.