Polycystic Ovary Syndrome (PCOS) represents one of the most prevalent endocrine disorders among individuals of reproductive age, affecting approximately 8% to 13% of women worldwide according to the World Health Organization. While the condition is characterized by a spectrum of symptoms including irregular menstrual cycles, weight gain, and infertility, its dermatological manifestations—specifically hormonal acne—often serve as the most visible and psychologically distressing markers. Unlike standard adolescent acne, PCOS-driven acne is frequently resistant to conventional over-the-counter treatments, necessitating a sophisticated, multi-modal medical approach that addresses the underlying hormonal imbalances rather than merely treating the surface of the skin.
The pathophysiology of PCOS-related acne is rooted in a complex disruption of the endocrine system, primarily involving the hypothalamic-pituitary-ovarian axis. In a healthy physiological state, the pituitary gland regulates the secretion of luteinizing hormone (LH) and follicle-stimulating hormone (FSH) to maintain a balance of estrogen, progesterone, and androgens. In patients with PCOS, this signaling becomes erratic, often resulting in elevated levels of androgens, such as testosterone and androstenedione. These "male" sex hormones, which exist naturally in all women, become pathological when in excess, stimulating the sebaceous glands to produce an overabundance of sebum. This oily substance, combined with a higher rate of skin cell turnover, creates an ideal environment for Cutibacterium acnes bacteria to thrive, leading to the deep, painful cystic lesions characteristic of the condition.

The Evolution of PCOS Diagnosis and Treatment
The clinical understanding of PCOS has evolved significantly since it was first described as the Stein-Leventhal syndrome in 1935. Historically, the focus remained strictly on ovarian cysts and fertility. However, the 2003 Rotterdam Criteria expanded the diagnostic framework to include hyperandrogenism (clinical or biochemical) and ovulatory dysfunction. This shift allowed dermatologists to play a more significant role in the early detection of the syndrome.
Chronologically, the treatment of acne has moved through several distinct eras. The 1970s marked a turning point with the FDA approval of topical retinoids and, later, oral isotretinoin (Accutane). By the 1990s, the link between insulin resistance and androgen production became a focal point of research, leading to the integration of metabolic management into dermatological care. Today, the medical community advocates for a "global" treatment strategy that combines hormonal therapy, lifestyle modifications, and advanced topical pharmacology.
The Insulin-Androgen Connection and Dietary Influence
A critical component of PCOS-driven acne is hyperinsulinemia, a condition where the body produces excess insulin due to cellular resistance. High levels of insulin are known to stimulate the ovaries to produce even more testosterone and simultaneously decrease the production of sex hormone-binding globulin (SHBG), a protein that normally "mops up" excess testosterone in the blood. This creates a feedback loop that exacerbates skin inflammation and sebum production.
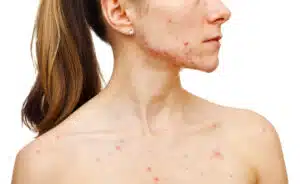
Clinical data suggests that dietary interventions are foundational to managing this metabolic aspect. Many nutritionists and endocrinologists recommend a Low Glycemic Index (GI) diet to stabilize blood sugar and insulin levels. Furthermore, emerging research has highlighted a potential link between dairy consumption and acne severity. Dairy products, particularly skim milk, have been shown to increase levels of insulin-like growth factor 1 (IGF-1), which further stimulates androgen production. For many patients with PCOS, the elimination of dairy can result in a noticeable reduction in inflammatory lesions within as little as two to four weeks, as the hormonal triggers for the sebaceous glands begin to subside.
Pharmacological Interventions: Retinoids and Isotretinoin
When dietary changes are insufficient, medical professionals often turn to retinoids, which are derivatives of Vitamin A. These compounds work by normalizing the way skin cells are shed, preventing the clogging of pores that initiates an acne flare. Topical retinoids, such as Tretinoin (Retin-A) or Adapalene (Differin), are considered first-line treatments for moderate acne.
For severe, recalcitrant cases, oral isotretinoin remains the "gold standard." However, its use in the PCOS population requires careful oversight. Isotretinoin targets all four causes of acne: excess sebum, clogged pores, bacteria, and inflammation. Despite its efficacy, the drug carries a significant risk profile, including potential liver toxicity, elevated cholesterol, and severe teratogenicity (risk of birth defects). In the United States, the iPLEDGE program mandates strict contraceptive measures for patients on isotretinoin. Furthermore, dermatologists note that while isotretinoin may clear skin temporarily, the underlying hormonal imbalance of PCOS may cause acne to return once the medication course is completed unless the hormonal drivers are addressed concurrently.

Antiandrogen Medications: Addressing the Root Cause
Because PCOS acne is fundamentally a result of androgen excess, antiandrogen medications are often utilized to block these hormones at the receptor level. Spironolactone, originally developed as a potassium-sparing diuretic to treat hypertension, has been used off-label for decades to treat hormonal acne and hirsutism (excessive hair growth) in women. By competing with androgens for binding sites on the sebaceous glands, Spironolactone effectively "mutes" the signal to produce oil.
Another antiandrogen, Cyproterone acetate, is frequently used internationally, often in combination with estrogen in oral contraceptives. Clinical trials have demonstrated that these medications can reduce acne by up to 50% to 80% within six months of consistent use. However, these treatments are not without side effects; Spironolactone can cause electrolyte imbalances and irregular spotting, while both require a commitment to long-term therapy, as symptoms typically return upon cessation.
The Role of Oral Contraceptives in Hormonal Stabilization
Hormonal birth control remains a primary tool in the management of PCOS. Combination pills containing both estrogen and progestin work by suppressing the ovaries’ production of androgens and increasing the levels of SHBG. This dual action significantly reduces the amount of free testosterone circulating in the bloodstream.
The FDA has specifically approved certain oral contraceptives, such as Yaz, Estrostep, and Ortho Tri-Cyclen, for the treatment of acne. However, medical providers must screen patients for contraindications. Individuals with PCOS are already at a higher risk for cardiovascular issues and metabolic syndrome; therefore, those who are obese, smoke, or have a history of blood clots (venous thromboembolism) may be advised against estrogen-containing pills. For those who can safely use them, these medications offer the benefit of regulating menstrual cycles while simultaneously clearing the skin.
Psychosocial Implications and Stress Management
The impact of PCOS acne extends beyond physical discomfort. Studies in the Journal of Clinical and Aesthetic Dermatology indicate that women with PCOS report higher rates of clinical depression, social anxiety, and reduced quality of life compared to the general population. The visible nature of acne, often occurring on the jawline, neck, and back, can lead to significant emotional distress.
This distress creates a biological feedback loop. Stress triggers the adrenal glands to release cortisol and dehydroepiandrosterone sulfate (DHEA-S), an adrenal androgen. In a patient with PCOS, this additional androgenic load can trigger new breakouts, creating a "stress-acne cycle." Consequently, the American Academy of Dermatology emphasizes the importance of stress-reduction techniques—such as mindfulness-based stress reduction (MBSR), regular physical activity, and cognitive-behavioral therapy—as adjuncts to medical treatment. These practices help lower systemic inflammation and mitigate the adrenal contribution to the syndrome.

Broader Impact and Future Outlook
The management of PCOS hormonal acne is an evolving field that increasingly prioritizes personalized medicine. As the medical community moves toward a better understanding of the genetic markers associated with PCOS, future treatments may involve targeted gene therapies or more sophisticated insulin-sensitizing agents that carry fewer side effects than current options like Metformin.
The broader implication for public health is clear: acne in adult women should not be dismissed as a cosmetic concern. It is frequently the "canary in the coal mine" for systemic endocrine dysfunction. Early intervention not only improves dermatological outcomes but also allows for the management of long-term risks associated with PCOS, including Type 2 diabetes, endometrial cancer, and cardiovascular disease. By integrating dermatological care with endocrinology and nutritional science, healthcare providers can offer a comprehensive pathway toward skin clarity and overall metabolic health for those living with Polycystic Ovary Syndrome.