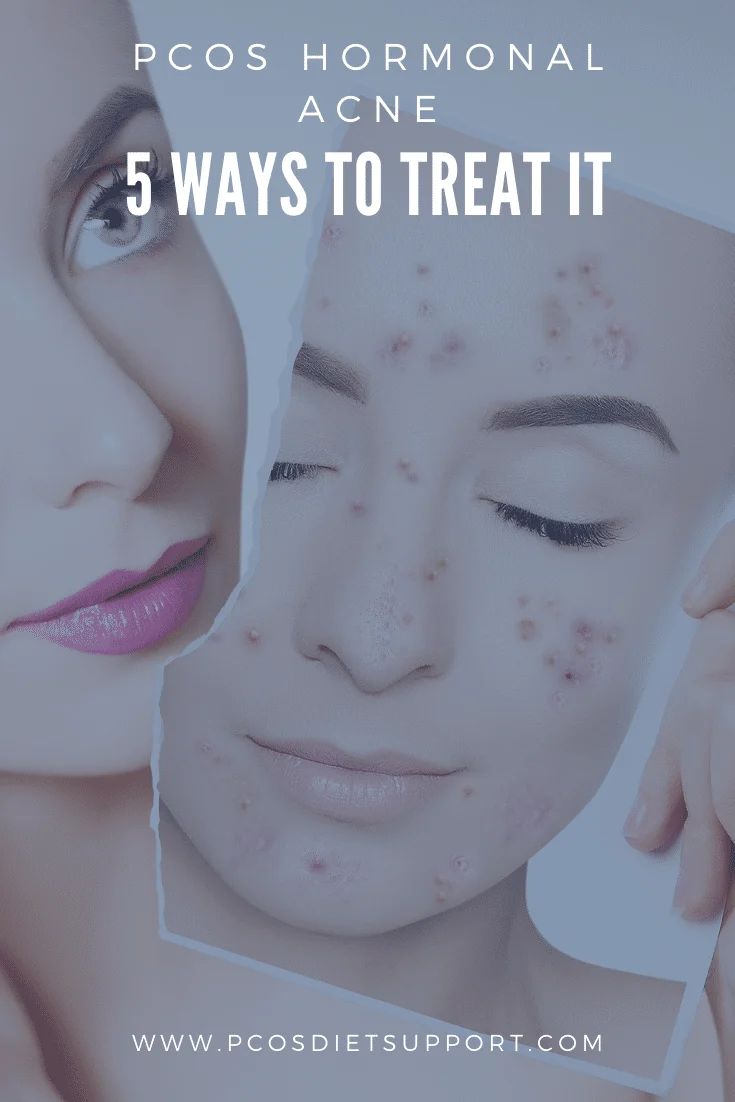
Polycystic Ovary Syndrome (PCOS) represents one of the most prevalent endocrine disorders among women of reproductive age, affecting an estimated 5% to 15% of the global population. While the condition is primarily defined by ovulatory dysfunction and polycystic ovarian morphology, its dermatological manifestations—specifically hormonal acne—often serve as the most visible and psychologically distressing symptoms. Unlike the transient breakouts associated with a typical menstrual cycle, PCOS-driven acne is characterized by its persistence, its resistance to standard over-the-counter treatments, and its tendency to flare along the jawline, chin, and neck. Understanding the complex interplay between the endocrine system and the skin’s sebaceous glands is critical for developing an effective, long-term management strategy that moves beyond topical applications to address the underlying hormonal drivers.
The Pathophysiology of PCOS-Related Acne
The development of acne in the context of PCOS is rarely a localized skin issue; rather, it is a symptom of a systemic hormonal imbalance rooted in the Hypothalamic-Pituitary-Ovarian (HPO) axis. Under normal physiological conditions, the pituitary gland regulates the production of estrogen, progesterone, and androgens. In a healthy cycle, these hormones fluctuate in a predictable rhythm to facilitate ovulation and menstruation. However, in women with PCOS, this feedback loop is disrupted. The pituitary gland often produces elevated levels of luteinizing hormone (LH), which stimulates the ovaries to produce excess androgens, most notably testosterone.

While androgens are often classified as "male" hormones, they are essential in women for maintaining bone density and reproductive tissue health. However, when androgen levels become pathologically elevated, they stimulate the sebaceous glands in the skin to produce excessive sebum (oil). This overproduction of oil, combined with a process called follicular hyperkeratosis—where skin cells do not shed properly and instead clog pores—creates the perfect environment for the bacterium Cutibacterium acnes to thrive. This leads to the deep, painful cystic lesions that are a hallmark of PCOS. Furthermore, many women with PCOS suffer from hyperinsulinemia, or high levels of insulin in the blood. Research indicates that insulin acts synergistically with LH to further drive androgen production in the ovaries and decreases the levels of Sex Hormone-Binding Globulin (SHBG), a protein that normally "mops up" excess testosterone in the blood. This dual mechanism ensures that more free testosterone is available to aggravate the skin.
Clinical Chronology: The Journey from Puberty to Diagnosis
The timeline for PCOS hormonal acne often begins in late adolescence or early adulthood. While many teenagers experience "common" acne (acne vulgaris) during puberty, those with PCOS find that their skin issues do not resolve as they enter their twenties. Instead, the breakouts may intensify. A typical clinical chronology involves a patient attempting various high-street benzoyl peroxide or salicylic acid treatments with little to no success.
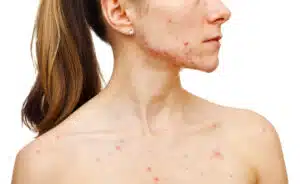
By the time a patient consults a dermatologist or endocrinologist, the acne has often become a chronic inflammatory condition. Medical professionals typically look for a pattern of symptoms: acne concentrated on the lower third of the face, hirsutism (excessive hair growth on the face or body), and irregular menstrual cycles. If two of these symptoms are present along with polycystic ovaries on an ultrasound, a diagnosis is made according to the Rotterdam Criteria, the international standard for PCOS diagnosis. This diagnosis marks a shift in treatment from purely cosmetic interventions to pharmacological and lifestyle-based strategies.
Pharmacological Interventions: Retinoids and Isotretinoin
When topical washes fail, the first line of clinical defense often involves retinoids. These derivatives of Vitamin A are foundational in dermatology because they regulate epithelial cell growth and prevent the clogging of pores. Prescription-strength topical retinoids, such as Tretinoin or Adapalene, work by increasing cell turnover, ensuring that dead skin cells are shed before they can trap sebum.
For severe or treatment-resistant cases, doctors may prescribe Isotretinoin, commonly known by the brand name Accutane. This oral medication is highly effective because it addresses all four causes of acne: excess oil production, clogged pores, bacteria, and inflammation. A standard course of Isotretinoin typically lasts 15 to 20 weeks, with dosages adjusted based on the patient’s body weight. However, the use of Isotretinoin in women with PCOS requires rigorous oversight. The drug is highly teratogenic, meaning it can cause severe birth defects if a patient becomes pregnant while taking it. Consequently, patients are often required to participate in the iPLEDGE program, which mandates the use of two forms of contraception and monthly pregnancy tests. While Isotretinoin can provide long-term remission for many, it does not cure the underlying hormonal imbalance of PCOS, meaning acne can potentially return once the medication is discontinued if the hormones remain unregulated.
Hormonal Regulation through Oral Contraceptives
Because the root of the problem is endocrine-based, many physicians recommend oral contraceptive pills (OCPs) as a primary treatment for PCOS symptoms. Combined oral contraceptives containing both estrogen and progestin are particularly effective. The estrogen component increases the liver’s production of SHBG, which binds to free testosterone, preventing it from interacting with the sebaceous glands. Meanwhile, the progestin suppresses the LH and FSH (follicle-stimulating hormone) pulses from the pituitary gland, effectively "quieting" the ovaries’ androgen production.

The American College of Obstetricians and Gynecologists (ACOG) notes that while OCPs are highly effective for cycle regulation and acne control, they are not suitable for everyone. Women who are obese, smokers over the age of 35, or those with a history of migraines with aura or blood clots are at an increased risk of deep vein thrombosis (DVT) when taking combined pills. Furthermore, medical experts emphasize that birth control functions as a symptomatic "mask." It manages the acne by providing synthetic hormones, but it does not address the metabolic issues—such as insulin resistance—that often drive PCOS.
The Role of Antiandrogens: Spironolactone and Cyproterone
For women who cannot take birth control or who require additional support, antiandrogen medications offer a targeted approach. Spironolactone, originally developed as a potassium-sparing diuretic for blood pressure management, has been used "off-label" in dermatology for over three decades. It works by blocking androgen receptors in the skin, ensuring that even if testosterone levels are high, the skin cannot "receive" the signal to produce more oil.
Another option is Cyproterone acetate, a progestogen with potent antiandrogenic properties. Often prescribed in combination with estrogen, it has a long history of success in reducing hirsutism and inflammatory acne. Data from clinical trials suggest that antiandrogens can reduce acne severity by up to 50% to 90% in women with PCOS, though results typically take three to six months to become visible.
Nutritional Science and the Insulin Connection
In recent years, the medical community has increasingly recognized the impact of diet on PCOS pathology. The "insulin-androgen" axis suggests that managing blood sugar is just as important as managing hormones. High-glycemic diets—those rich in refined sugars and white flours—trigger rapid insulin spikes, which directly stimulate the ovaries to produce more testosterone.
Dairy consumption has also come under scrutiny. Several studies have identified a link between dairy intake and acne severity, hypothesized to be due to the presence of insulin-like growth factor 1 (IGF-1) in cow’s milk. IGF-1 can stimulate the sebaceous glands and increase the sensitivity of the skin to androgens. Many women with PCOS report significant improvements in skin clarity within weeks of eliminating dairy and adopting a low-glycemic, anti-inflammatory diet. This nutritional approach focuses on whole foods, fiber, and healthy fats, which help stabilize insulin levels and, by extension, androgen levels.
Broader Impact: Psychological Well-being and Stress Management
The implications of PCOS hormonal acne extend far beyond physical appearance. The chronic nature of the condition is frequently linked to lower self-esteem, social withdrawal, and higher rates of anxiety and depression. This creates a physiological "vicious cycle." Stress triggers the adrenal glands to produce cortisol and DHEA-S (another androgen), which can further exacerbate acne breakouts.

Professional psychological support and stress-reduction techniques, such as mindfulness, yoga, and regular physical activity, are now considered essential components of a holistic PCOS treatment plan. By managing the body’s stress response, patients can help lower the systemic inflammation that contributes to cystic acne.
Conclusion and Future Outlook
Managing PCOS hormonal acne requires a multidisciplinary approach that bridges the gap between dermatology, endocrinology, and nutrition. While topical treatments and retinoids can address the surface-level symptoms, long-term success is usually found through the regulation of androgens and insulin. As research continues to evolve, the focus is shifting toward more personalized medicine, where genetic markers and specific metabolic profiles guide treatment choices. For the millions of women living with PCOS, the transition from reactive skincare to proactive endocrine management offers not only the hope of clearer skin but also a path toward better overall systemic health.