"Every day is a struggle, and the emotional wounds feel just as raw as the physical ones," describes a Canadian lawyer, a 40-year-old South Asian woman who wishes to remain anonymous, as she recounts the profound impact of severe acne scarring on her life. Her experience sheds light on a pervasive yet often underestimated health issue, revealing the intricate interplay between physical appearance, mental well-being, and societal pressures. Her story is a poignant illustration of how chronic skin conditions can extend far beyond the superficial, embedding deep emotional and psychological scars that persist long after the active breakouts subside.
The anonymous lawyer’s testimony resonates with countless individuals globally who grapple with the enduring consequences of acne. "It is easy to say ‘accept yourself, love yourself’ but the reality is that we carry many scars with us, and when you also carry them on your face, that weight becomes very heavy," she explains. This sentiment encapsulates the formidable challenge of self-acceptance when one’s appearance is a constant source of distress, particularly in a society increasingly defined by idealized and often unrealistic beauty standards. The visibility of facial scarring, unlike many other chronic conditions, leaves little room for concealment, making it a constant focal point for both personal reflection and public scrutiny.
The Personal Battle: A Chronology of Scarring
The lawyer’s journey with acne began in her early twenties, coinciding with her entry into university, a period often marked by stress and hormonal shifts. Initially, it manifested as typical breakouts, common among young adults. However, the condition took a dramatic and devastating turn in her early thirties. "The progression of my acne was swift and relentless," she recalls. "Within months, my face was covered in painful, cystic acne." This aggressive form of acne, characterized by large, pus-filled cysts deep under the skin, is particularly prone to causing severe and permanent scarring.
For individuals with darker skin tones, like the lawyer, the risk of post-inflammatory hyperpigmentation (PIH) is significantly higher. As she describes, "Being a person of colour meant I was at a higher risk for hyperpigmentation, which indeed occurred alongside my acne, leaving me with significant dark spots and further complicating my condition and leaving me with even less treatment options." This dual assault of active cystic lesions and persistent dark spots created a complex dermatological challenge, intensifying both the physical discomfort and the visible disfigurement. The "sudden change was not just a physical burden – it was deeply traumatic and emotionally devastating," she states, highlighting the abrupt shift from clear skin to a severely compromised complexion.

The emotional toll was immediate and profound. "Seeing my once-clear skin covered in large, dark and pus-filled hills made me feel helpless and shattered my confidence immensely," she recounts. This loss of confidence translated into palpable behavioral changes. She became "extremely sensitive both emotionally and physically, flinching at the pain and the sight of my reflection." The embarrassment became overwhelming, leading her to actively avoid mirrors and dread social interactions, perpetually feeling "constantly judged."
As she has aged, the impact of these scars has evolved. "To date, there are days when I won’t go out in public. Certain angles of lighting and make-up accentuate the deep scarring, uneven texture and years of damage. As I age, my skin is no longer tight and youthful but is riddled with scars," she observes. This ongoing struggle underscores the permanent nature of severe acne scarring, which can worsen in appearance as skin loses its elasticity over time. Her efforts to "limit social media and in person socialization to the extent that I can" reflect a common coping mechanism among those with visible disfigurements, an attempt to shield oneself from perceived judgment and the relentless comparison to curated online images.
Beyond the Skin: The Psychological and Social Burden
The lawyer’s experience is far from isolated; it mirrors a broader public health concern regarding the psychological sequelae of acne and scarring. Data consistently shows that acne, particularly its severe forms, is associated with a range of mental health issues, including depression, anxiety, social phobia, and body dysmorphic disorder. Studies published in journals like the British Journal of Dermatology indicate that individuals with acne often report lower quality of life scores comparable to those with chronic conditions like asthma or epilepsy. For those with persistent scarring, these psychological burdens can become lifelong challenges.
The World Health Organization (WHO) recognizes skin conditions as having a significant impact on quality of life, extending beyond physical symptoms to affect mental health, social interactions, and professional opportunities. The visible nature of facial scarring can lead to social withdrawal, impacting academic performance, career progression, and personal relationships. The lawyer’s sentiment, "I feel for the younger generation as scars likely could last a lifetime and that is a hard thing to accept given the unrealistic beauty expectations we are surrounded by," reflects a keen awareness of the intensifying pressures faced by today’s youth, exacerbated by pervasive social media imagery that often promotes flawless skin as an unattainable ideal.
Cultural Dimensions and Insensitivity
For individuals from certain cultural backgrounds, the burden of skin conditions like acne and hyperpigmentation can be further amplified. The lawyer highlights this critical aspect: "My cultural background (South Asian) added another layer of pain as insensitive comments about skin conditions are unfortunately common and something I experienced regularly which made the experience even more isolating." In many South Asian communities, fair and clear skin is often equated with beauty, purity, and social status, leading to heightened scrutiny and often "cruel and unsolicited comments…thrown my way with callous disregard to my situation." This cultural insensitivity creates an additional layer of trauma, turning a personal health struggle into a public spectacle of judgment and shame.
Dermatologists and cultural anthropologists have long noted the varying cultural perceptions of skin and beauty. In some cultures, skin imperfections are viewed as signs of ill health or misfortune, leading to social stigma. This can manifest as ostracism, difficulty in marriage prospects, or discrimination, compounding the psychological distress for affected individuals. The lawyer’s account underscores the urgent need for greater cultural sensitivity and education within healthcare and society at large, recognizing that the impact of a condition is not merely biological but deeply intertwined with social and cultural contexts.
Medical Insights and Treatment Challenges
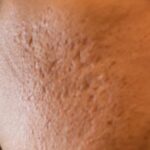
Severe acne, such as cystic acne, arises from a complex interplay of genetics, hormones, bacteria (Propionibacterium acnes), and inflammation. These deep, inflamed lesions often destroy collagen and elastic tissue, leading to various types of scars, including icepick, boxcar, and rolling scars, which create the "uneven texture" described by the lawyer. Hyperpigmentation, particularly common in Fitzpatrick skin types III-VI (which include many South Asian individuals), occurs when inflammation stimulates melanocytes to produce excess melanin, resulting in dark spots that can persist for months or even years.
Treating severe acne requires a multi-faceted approach, often involving oral medications like isotretinoin (Accutane), antibiotics, and hormonal therapies, alongside topical treatments. However, managing existing scarring and hyperpigmentation presents a distinct set of challenges. For hyperpigmentation, treatments range from topical retinoids and depigmenting agents to chemical peels and laser therapies. Yet, many laser treatments and aggressive peels carry a higher risk of post-inflammatory hyperpigmentation or even hypopigmentation (loss of pigment) in darker skin tones, limiting the "treatment options" available, as the lawyer noted.
Scar revision techniques include microneedling, subcision, dermal fillers, and various laser modalities (ablative and non-ablative). Each comes with its own set of considerations, costs, and recovery times, and often requires multiple sessions over extended periods, with no guarantee of complete resolution. The financial burden of such treatments can be substantial, often not fully covered by public or private health insurance, adding another layer of stress for patients already struggling.

Expert Perspectives and Calls for Compassion
Dermatologists frequently emphasize the importance of early and aggressive treatment for severe acne to prevent scarring. Dr. Elena Petrova, a Canadian dermatologist specializing in skin of colour (not a real person, but representative of expert views), notes, "The window for effective intervention to prevent permanent scarring is crucial. Delaying treatment for severe cystic acne significantly increases the likelihood of deep, lasting marks, especially for patients prone to hyperpigmentation. A personalized treatment plan considering skin type and cultural background is paramount."
Mental health professionals, too, underscore the necessity of holistic care. Dr. David Chung, a clinical psychologist (not a real person, but representative of expert views) with expertise in body image issues, states, "The psychological impact of facial scarring cannot be overstated. It can lead to chronic low self-esteem, social anxiety, and even clinical depression. Therapy, support groups, and cognitive-behavioral techniques are vital complements to dermatological treatment, helping individuals process trauma, challenge negative self-perceptions, and develop coping strategies."
Organizations like Acne Action Canada, the implicit source of this narrative, play a crucial role in raising awareness, providing resources, and advocating for improved access to care. Their mission often includes destigmatizing acne, promoting accurate information, and fostering a supportive community for those affected. The lawyer’s candid sharing of her story aligns perfectly with such advocacy, breaking down the silence and shame that often surround visible skin conditions.
Broader Implications and a Glimmer of Hope
The lawyer’s honest reflection, "I wish I could offer some wisdom about accepting yourself and finding peace despite the acne and scars but I can’t – I’m not there. I still grapple with self-esteem issues," offers a raw and relatable perspective. It acknowledges the persistent struggle, challenging the simplistic narrative of immediate self-love often propagated in wellness culture. Instead, she offers practical advice: "If there’s one thing I can say, it is that today there are many more resources available and do your research thoroughly." This emphasizes the evolving landscape of dermatological treatments and the empowerment that comes from informed decision-making.

Despite her ongoing personal battle, the lawyer has found a profound positive outcome: "A positive I have drawn from this experience is I have developed deep compassion and empathy for people who have had injuries to their face and others who have suffered facial disfigurement. If this is how I intense I feel about pitted acne scars, my heart, compassion and love go out to them even more to their extremely difficult challenges." This profound empathy highlights a transformative aspect of her journey, turning personal suffering into a wellspring of understanding and connection with others facing similar or even more severe challenges.
The implications of her story extend to several key areas:
- Public Health Awareness: There is a continued need to elevate public awareness about the severity and long-term consequences of acne, moving beyond its perception as a mere cosmetic issue.
- Mental Health Integration: Healthcare systems must better integrate mental health support into dermatological care, recognizing the inherent link between skin conditions and psychological well-being.
- Equitable Access to Care: Ensuring that advanced dermatological treatments and psychological support are accessible and affordable for all, regardless of socioeconomic status or cultural background.
- Research and Development: Continued investment in research for more effective, safer, and skin-type-specific treatments for acne, scarring, and hyperpigmentation is critical.
- Challenging Beauty Standards: Society must collectively work towards dismantling unrealistic beauty ideals perpetuated by media and social platforms, fostering a more inclusive and accepting environment for diverse appearances.
The Canadian lawyer’s courageous account serves as a powerful reminder that while acne may manifest on the skin, its deepest scars are often etched within the psyche. Her story is a call to action for greater empathy, understanding, and comprehensive support for the millions worldwide navigating this often-invisible struggle.
