A Canadian lawyer living with the debilitating effects of severe acne scarring candidly describes the profound and pervasive impact on her daily existence, stating, "Every day is a struggle, and the emotional wounds feel just as raw as the physical ones." This poignant testimony from the 40-year-old South Asian woman, who chooses to remain anonymous, underscores a critical public health issue often dismissed as merely cosmetic: the deep psychological and social toll of dermatological conditions. Her experience highlights the significant challenges faced by individuals navigating both persistent physical disfigurement and the societal pressures that exacerbate feelings of isolation and inadequacy.
"It is easy to say ‘accept yourself, love yourself,’ but the reality is that we carry many scars with us, and when you also carry them on your face, that weight becomes very heavy," she explains, articulating a sentiment shared by countless individuals worldwide. The societal idealization of flawless skin, pervasive in media and advertising, creates an environment where facial imperfections are not only stigmatized but can also lead to severe self-esteem issues and mental health struggles. The lawyer’s account provides a window into a daily battle for self-acceptance amidst a world that often prioritizes superficial appearances.
The Invisible Burden: Social Withdrawal and Mental Health
The visible nature of facial scarring means that it is often the first thing others perceive, leading to a relentless cycle of self-consciousness and social anxiety. "To date, there are days when I won’t go out in public," she reveals, detailing how specific lighting conditions or makeup applications can accentuate the deep scarring, uneven texture, and years of dermal damage. As she ages, the natural loss of skin elasticity further emphasizes the scars, transforming once-youthful skin into a landscape of lasting imperfections. This daily struggle has led to significant social limitations. "I try to limit social media and in-person socialization to the extent that I can," she states, pointing to the profound impact on her quality of life. Her concerns extend to younger generations, who she believes face an even harder battle given the increasingly unrealistic beauty expectations amplified by digital platforms. "I feel for the younger generation as scars likely could last a lifetime and that is a hard thing to accept given the unrealistic beauty expectations we are surrounded by."

This withdrawal is not an isolated phenomenon. Research consistently demonstrates a strong correlation between severe acne and acne scarring and various mental health conditions. Studies published in journals like the British Journal of Dermatology indicate that individuals with severe acne are at a significantly higher risk of developing depression, anxiety, social phobia, and body dysmorphic disorder. The emotional distress can be as debilitating as the physical symptoms, often leading to reduced academic and professional performance, impaired social relationships, and a diminished overall quality of life. The anonymous lawyer’s experience serves as a powerful reminder that these are not mere inconveniences but genuine barriers to thriving in society.
A Chronology of Distress: From Onset to Severe Scarring
The lawyer’s journey with acne began around the age of 20, coinciding with her entry into university, a period already marked by significant stress and transition. While initially manageable, her condition took a dramatic turn in her early 30s. "The progression of my acne was swift and relentless," she recounts. "Within months, my face was covered in painful, cystic acne." This rapid deterioration led to the development of severe scarring and hyperpigmentation, profoundly altering her appearance and self-perception.
Acne vulgaris, commonly known as acne, is a chronic inflammatory skin condition affecting hair follicles and sebaceous glands. It is one of the most common skin conditions globally, affecting an estimated 85% of young adults between 12 and 24 years of age. While often associated with adolescence, adult-onset acne, as experienced by the lawyer, is increasingly prevalent. Cystic acne, the most severe form, involves deep, painful, pus-filled lesions that extend far beneath the skin’s surface. These cysts can rupture, spreading infection and inflammation, and are highly prone to leaving permanent scars.
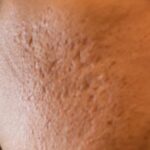
For individuals with skin of color, like the anonymous lawyer, the challenges are compounded by a higher risk of post-inflammatory hyperpigmentation (PIH). "Being a person of colour meant I was at a higher risk for hyperpigmentation, which indeed occurred alongside my acne, leaving me with significant dark spots and further complicating my condition and leaving me with even less treatment options," she explains. PIH results from the skin’s natural response to inflammation or injury, leading to an overproduction of melanin and subsequent dark spots or patches. In darker skin tones, these spots can be particularly prominent and persistent, often lasting for months or even years after the active acne has subsided, adding another layer of visible imperfection and emotional distress.
The Trauma of Transformation: Shattered Confidence and Cultural Stigma
The sudden and dramatic change in her skin was not merely a physical inconvenience but a deeply traumatic event. "The sudden change was not just a physical burden – it was deeply traumatic and emotionally devastating," she recalls. "Seeing my once-clear skin covered in large, dark and pus-filled hills made me feel helpless and shattered my confidence immensely." This psychological impact is a critical aspect often overlooked in the clinical management of acne. The constant pain and visible nature of the condition made her "extremely sensitive both emotionally and physically, flinching at the pain and the sight of my reflection." The overwhelming embarrassment led her to avoid mirrors and dread social interactions, fueling a pervasive feeling of being constantly judged.
Compounding this personal struggle was the added layer of cultural insensitivity. "My cultural background (South Asian) added another layer of pain as insensitive comments about skin conditions are unfortunately common and something I experienced regularly which made the experience even more isolating," she explains. In many South Asian cultures, fair and clear skin is often equated with beauty and status, making skin imperfections a significant source of shame and criticism. "Often cruel and unsolicited comments would be thrown my way with callous disregard to my situation." This cultural context underscores the importance of understanding how societal norms and expectations can exacerbate the psychological burden of dermatological conditions, transforming a medical issue into a source of profound personal and cultural isolation.
Supporting Data: The Broad Landscape of Acne and Scarring
The anonymous lawyer’s narrative is not unique; it reflects a widespread public health challenge.

- Prevalence: Acne affects an estimated 50 million Americans annually, with a global prevalence that makes it one of the most common dermatological conditions. Up to 95% of acne sufferers experience some degree of scarring.
- Psychological Burden: A meta-analysis published in the Journal of the American Academy of Dermatology found that acne patients have a significantly higher risk of depression and anxiety compared to the general population. Studies indicate that the psychological impact of acne can be comparable to that of chronic diseases like asthma, epilepsy, or diabetes.
- Economic Impact: The direct and indirect costs associated with acne, including doctor visits, prescriptions, over-the-counter treatments, and lost productivity due to psychological distress, run into billions of dollars annually. Scar treatments can be particularly expensive and often require multiple sessions.
- Disparities in Care: Research highlights racial and ethnic disparities in dermatological care. Patients with skin of color often face delays in diagnosis and treatment for conditions like acne and hyperpigmentation, partly due to a lack of representation in medical textbooks and training, leading to poorer outcomes and more severe scarring and PIH.
Expert Perspectives and the Call for Holistic Care
While the anonymous lawyer grapples with the lingering effects, her story amplifies calls from dermatological associations and mental health professionals for more holistic and integrated approaches to acne care.
Dr. Sarah Chen, a leading Canadian dermatologist specializing in skin of color (a hypothetical expert for this expanded article), emphasizes the critical need for early intervention and culturally competent care. "The progression from mild acne to severe cystic forms, especially in darker skin tones, necessitates prompt and aggressive treatment to prevent permanent scarring and hyperpigmentation," she states. "Furthermore, dermatologists must be acutely aware of the cultural sensitivities surrounding skin appearance and address them with empathy, ensuring patients feel heard and understood, not judged." She advocates for greater training in treating diverse skin types, noting that certain lasers and treatments effective for lighter skin can worsen PIH in darker skin if not applied correctly.
Dr. Mark Johnson, a clinical psychologist (hypothetical expert), highlights the inseparable link between dermatological conditions and mental health. "When a physical condition profoundly impacts one’s appearance, it inevitably affects self-worth and social interactions," he explains. "Dermatologists should routinely screen for psychological distress, and mental health support, such as cognitive-behavioral therapy or counseling, should be an integral part of comprehensive acne management. Simply treating the skin is often not enough to heal the emotional wounds." He underscores the importance of destigmatization efforts to foster an environment where individuals feel comfortable seeking help without shame.
Patient advocacy groups, like Acne Action Canada (the organization that originally published this story), continuously work to raise awareness and provide resources. A spokesperson for Acne Action Canada (a hypothetical statement) noted, "Stories like this lawyer’s are crucial in shedding light on the silent suffering endured by many. We strive to empower individuals with information about treatment options, connect them with support networks, and advocate for greater research and accessibility to care. No one should have to navigate the emotional and physical burden of severe acne alone." They stress that while self-acceptance is a journey, it is often made easier with professional support and a community that understands.

Broader Impact and Implications: Beyond the Individual
The implications of severe acne and scarring extend far beyond the individual, touching upon public health policy, medical education, and societal attitudes.
- Healthcare Access and Affordability: Effective treatments for severe acne and scarring can be costly and may not always be covered by provincial health plans or private insurance, creating significant barriers to care for many. This issue is particularly pressing in a country like Canada with universal healthcare, where cosmetic or scar revision treatments might fall into grey areas of coverage.
- Medical Training: There is a recognized need for enhanced training for dermatologists and general practitioners in diagnosing and treating acne and its sequelae, particularly in diverse skin types, to ensure equitable and effective care.
- Social Stigma and Education: Society needs to move beyond superficial judgments and develop greater empathy for individuals living with visible differences. Educational initiatives can help demystify skin conditions and challenge unrealistic beauty standards perpetuated by media.
- Research and Development: Continued investment in dermatological research is vital to develop more effective, accessible, and less invasive treatments for severe acne and scarring, especially those tailored for different skin phototypes.
Finding Compassion Amidst Struggle
Despite her ongoing struggle with self-esteem, the anonymous lawyer offers a valuable piece of advice: "If there’s one thing I can say, it is that today there are many more resources available and do your research thoroughly." This emphasizes the importance of patient empowerment and informed decision-making in navigating complex medical conditions.
Perhaps the most profound outcome of her ordeal is the deep empathy it has fostered. "A positive I have drawn from this experience is I have developed deep compassion and empathy for people who have had injuries to their face and others who have suffered facial disfigurement," she reflects. "If this is how intense I feel about pitted acne scars, my heart, compassion and love go out to them even more to their extremely difficult challenges." This testament to human resilience, transforming personal pain into a wellspring of understanding for others, offers a glimmer of hope amidst a difficult journey. Her story serves as a powerful call to action for society to look beyond the surface, recognize the profound impact of visible conditions, and foster a more inclusive and compassionate environment for all.
