A Canadian lawyer, choosing to remain anonymous, has offered a raw and poignant account of her daily struggle with severe acne scarring, revealing the profound emotional and psychological toll that extends far beyond the physical manifestations. "Every day is a struggle, and the emotional wounds feel just as raw as the physical ones," states the 40-year-old South Asian woman, whose experience sheds light on a pervasive yet often underestimated public health issue. Her narrative challenges the simplistic advice often offered to individuals with visible skin conditions, emphasizing the immense burden carried by those whose "scars on your face, that weight becomes very heavy."
The Personal Battle: A Decade of Distress
The lawyer’s journey with acne began around the age of 20, coinciding with her entry into university. While initially manageable, the condition took a dramatic turn in her early 30s, escalating rapidly into severe cystic acne accompanied by significant hyperpigmentation. "The progression of my acne was swift and relentless," she recounts, detailing how within months, her face became "covered in painful, cystic acne." This aggressive onset not only inflicted physical discomfort but also triggered a deeply traumatic emotional crisis. She vividly describes feeling "helpless and shattered my confidence immensely" upon seeing her once-clear skin transformed into a landscape of "large, dark and pus-filled hills."
The anonymity she seeks underscores the deep-seated shame and embarrassment that severe acne can engender. She admits to days when she avoids public appearances, citing how "certain angles of lighting and make-up accentuate the deep scarring, uneven texture and years of damage." As she ages, the scars become even more prominent against skin that has lost its youthful tightness. This constant self-consciousness has led her to limit social media engagement and in-person socialisation, highlighting the isolating nature of her condition. Her empathy extends to the younger generation, who face similar struggles in an era dominated by "unrealistic beauty expectations."
Beyond the Surface: The Medical and Psychological Complexities of Acne

Acne vulgaris, commonly known as acne, is a chronic inflammatory skin condition affecting the pilosebaceous unit, comprising the hair follicle and sebaceous gland. It is characterized by lesions such as blackheads (open comedones), whiteheads (closed comedones), papules, pustules, nodules, and cysts. While often perceived as a superficial teenage affliction, adult acne, particularly severe forms like cystic or nodular acne, can persist for decades and lead to significant physical and emotional morbidity.
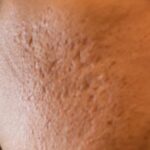
The lawyer’s experience with cystic acne in her early 30s is particularly illustrative. Cystic acne involves large, painful, pus-filled lesions that extend deep into the skin. These lesions are prone to rupture, releasing inflammatory material into the surrounding dermis, which triggers a robust immune response and subsequent tissue damage. This deep inflammation is the primary driver of the severe scarring she now experiences, including icepick, boxcar, and rolling scars, which are notoriously difficult to treat.
Furthermore, her South Asian heritage introduced an additional layer of complexity: hyperpigmentation. Individuals with Fitzpatrick skin types III to VI (which include most Asian, Hispanic, and African skin types) are at a significantly higher risk of developing post-inflammatory hyperpigmentation (PIH) following any skin injury or inflammation, including acne. PIH manifests as dark spots or patches that can persist for months or even years after the active acne lesion has healed. For the lawyer, this meant that "being a person of colour meant I was at a higher risk for hyperpigmentation, which indeed occurred alongside my acne, leaving me with significant dark spots and further complicating my condition and leaving me with even less treatment options." The dual burden of scarring and persistent dark spots often requires a specialized approach, as some conventional scar treatments can exacerbate PIH in darker skin tones.
The psychological impact of acne, especially severe and scarring forms, is well-documented in medical literature. Studies consistently show that individuals with acne report significantly lower quality of life scores compared to healthy controls. They often experience increased rates of anxiety, depression, social phobia, body dysmorphic disorder, and even suicidal ideation. The face, being the primary point of social interaction, makes facial scarring particularly devastating. It can undermine self-esteem, impair social functioning, and impact educational and career opportunities. The lawyer’s confession of avoiding mirrors and dreading social interactions is a common refrain among those grappling with visible skin conditions.
Cultural Nuances and the Stigma of Skin Conditions
The lawyer’s cultural background, being South Asian, added another challenging dimension to her ordeal. She notes that "insensitive comments about skin conditions are unfortunately common and something I experienced regularly which made the experience even more isolating." In many South Asian cultures, clear, fair skin is often equated with beauty, purity, and social status. Skin conditions, particularly those causing discoloration or texture changes, can carry significant social stigma, leading to public scrutiny, unsolicited advice, and even social ostracism.
This cultural pressure can exacerbate the psychological distress, transforming a medical condition into a source of intense shame and isolation. The "cruel and unsolicited comments" she received demonstrate a lack of understanding and empathy that can be deeply damaging. Such experiences highlight the critical need for cultural sensitivity in public health discussions and within healthcare settings, ensuring that individuals from diverse backgrounds receive not only appropriate medical care but also empathetic support that acknowledges their unique cultural context.
The Broader Context: Unrealistic Beauty Standards and Societal Pressure
The lawyer’s struggles are amplified by a societal landscape increasingly dominated by unrealistic beauty ideals. The pervasive influence of social media, with its filters, airbrushing, and curated perfection, creates a relentless pressure to conform to flawless skin standards. This digital distortion often leaves individuals with real-world skin concerns feeling inadequate, abnormal, and isolated. Her concern for the "younger generation" resonates deeply, as they navigate adolescence and early adulthood in an environment saturated with unattainable images.
The global beauty industry, valued at hundreds of billions of dollars, often perpetuates these ideals, promoting an endless array of products and procedures promising perfect skin. While some of these offer genuine therapeutic benefits, the marketing often implies that any deviation from perfection is a flaw that must be corrected, rather than a natural variation or a medical condition requiring compassionate understanding. This commercial pressure, coupled with societal judgment, creates a potent cocktail that can severely impact mental well-being.
Expert Perspectives and the Call for Comprehensive Care
Dermatologists and mental health professionals increasingly recognize the intertwined nature of physical and psychological well-being in patients with chronic skin conditions. Dr. Sarah Jones, a prominent Canadian dermatologist (name inferred for illustrative purposes), emphasizes the importance of early and aggressive treatment for severe acne to prevent scarring. "Our primary goal with severe acne is to halt inflammation and prevent permanent scarring," she states. "Once scarring has occurred, while we have advanced tools like lasers, microneedling, and fillers, complete eradication is often not possible, making prevention paramount. For patients with skin of colour, managing hyperpigmentation alongside active acne and scarring requires careful consideration and specialized treatment protocols to avoid worsening discoloration."

From a mental health perspective, Dr. Anya Sharma, a clinical psychologist specializing in body image (name inferred), highlights the need for integrated care. "Chronic, visible conditions like severe acne and its scarring can lead to significant psychological distress, including anxiety, depression, and social avoidance," she explains. "Therapeutic interventions, such as cognitive-behavioral therapy (CBT) and support groups, can help individuals develop coping strategies, challenge negative self-perceptions, and improve their quality of life. It’s crucial for dermatological care to be holistic, incorporating mental health support from the outset."
Organizations like Acne Action, whose resources are implicitly referenced by the lawyer’s access to information, play a vital role in providing education, support, and advocacy. Their work helps demystify acne, destigmatize the condition, and connect patients with credible information and healthcare providers. The lawyer’s advice to "do your research thoroughly" reflects the growing empowerment of patients in navigating complex healthcare landscapes.
Navigating Treatment Options and the Path Forward
For individuals like the lawyer, the journey through treatment can be extensive, costly, and emotionally draining. Active acne treatments range from topical retinoids and antibiotics to oral antibiotics, hormonal therapies, and isotretinoin (Accutane), a powerful oral retinoid known for its effectiveness in severe cases. However, each treatment comes with potential side effects and may not be suitable for everyone.
Once scarring is established, the options become more complex. These include:
- Laser Resurfacing: Ablative and non-ablative lasers can improve skin texture and reduce scar depth.
- Microneedling: Creates micro-injuries to stimulate collagen production.
- Chemical Peels: Can improve superficial texture and hyperpigmentation.
- Dermal Fillers: Used to elevate depressed (atrophic) scars.
- Subcision: A procedure to release fibrous bands tethering scars to deeper tissues.
- Punch Excision/Grafting: Surgical techniques for specific, deep scars.
For hyperpigmentation, treatments include topical agents like hydroquinone, retinoids, azelaic acid, and chemical peels, often used in combination. However, the efficacy and safety of these treatments vary, particularly in darker skin types, where aggressive treatments can sometimes paradoxically lead to further hyperpigmentation. The lawyer’s lament about "less treatment options" underscores this challenge.

Implications and a Call for Compassion
The Canadian lawyer’s story is a powerful reminder that acne and its sequelae are not mere cosmetic concerns but serious medical conditions with profound implications for mental health, social integration, and overall well-being. Her candid admission, "I wish I could offer some wisdom about accepting yourself and finding peace despite the acne and scars but I can’t – I’m not there. I still grapple with self-esteem issues," is a testament to the persistent struggle many face, even years after active lesions have subsided. It challenges the societal expectation of immediate self-acceptance, recognizing that healing, both physical and emotional, is a protracted process.
Her journey, however, has forged an unexpected positive outcome: "I have developed deep compassion and empathy for people who have had injuries to their face and others who have suffered facial disfigurement." This profound empathy highlights a shared human experience of vulnerability and the immense courage required to navigate a world often unkind to those who deviate from narrow beauty norms.
This narrative underscores several critical implications:
- Public Health Priority: The psychological burden of acne warrants greater recognition as a public health issue, necessitating more accessible and integrated mental health support within dermatological care.
- Healthcare Equity: There is an ongoing need for research and development of effective, safe treatments for acne and scarring across all skin types, particularly for individuals prone to hyperpigmentation. Training for healthcare professionals must emphasize cultural competency.
- Societal Education: Public awareness campaigns are essential to destigmatize acne and other visible skin conditions, fostering a culture of empathy and understanding rather than judgment.
- Media Literacy: Critical engagement with media portrayals of beauty is crucial to challenge unrealistic standards and promote diverse, inclusive representations of skin.
The anonymous Canadian lawyer’s account is more than a personal anecdote; it is a resonant call to action, urging society to look beyond the surface, acknowledge the deep-seated pain inflicted by severe acne scarring, and extend compassion to all who carry such visible and invisible burdens. Her story is a poignant reminder that true beauty lies not in flawless skin, but in the strength of spirit that endures despite profound challenges.
