The World Health Organization has issued an urgent call to action for nations across the globe to accelerate their efforts in the fight against tuberculosis, a disease that remains one of the most significant threats to global public health. On World TB Day 2026, the organization emphasized that the eradication of this ancient disease is within reach, provided that governments prioritize the deployment of groundbreaking diagnostic innovations and ensure equitable access to treatment. Central to this new push are guidelines for point-of-care diagnostic tests and non-invasive sampling methods, such as tongue swabs, which are designed to reach the most vulnerable populations who have historically been underserved by traditional healthcare infrastructures.
Under the theme “Yes! We can end TB: Led by countries, powered by people,” the WHO is advocating for a paradigm shift in how the disease is managed. The focus has moved toward decentralizing care, moving diagnostic capabilities out of centralized laboratories and into the heart of communities. This strategy aims to close the persistent gap between the number of people falling ill and those receiving a formal diagnosis and subsequent treatment. By leveraging new technology that is both portable and affordable, the WHO believes the global community can finally reverse the trends of a disease that continues to claim thousands of lives every single day.
Breakthroughs in Point-of-Care Diagnostics
The cornerstone of the WHO’s 2026 strategy is the introduction of new guidelines for diagnostic tests that can be administered at the point-of-care. For decades, TB diagnosis relied heavily on sputum smear microscopy—a method that is over a century old and often lacks sensitivity—or expensive molecular tests that required stable electricity and sophisticated laboratory settings. The new generation of portable, battery-operated molecular tests represents a technological leap forward. These devices are capable of delivering highly accurate results in under an hour, a timeframe that allows healthcare providers to initiate treatment during the patient’s initial visit.
The economic implications of these tools are as significant as their clinical benefits. Available at less than half the cost of many previous molecular diagnostics, these tests lower the barrier to entry for low- and middle-income countries. Because they do not require a continuous connection to a power grid, they are uniquely suited for use in rural clinics, mobile health units, and conflict zones. Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, noted that these tools are transformative because they bring fast, accurate diagnosis directly to the people who need it most, thereby curbing transmission and reducing the long-term costs associated with untreated or late-diagnosed TB.
Innovations in Sample Collection: Tongue Swabs and Sputum Pooling
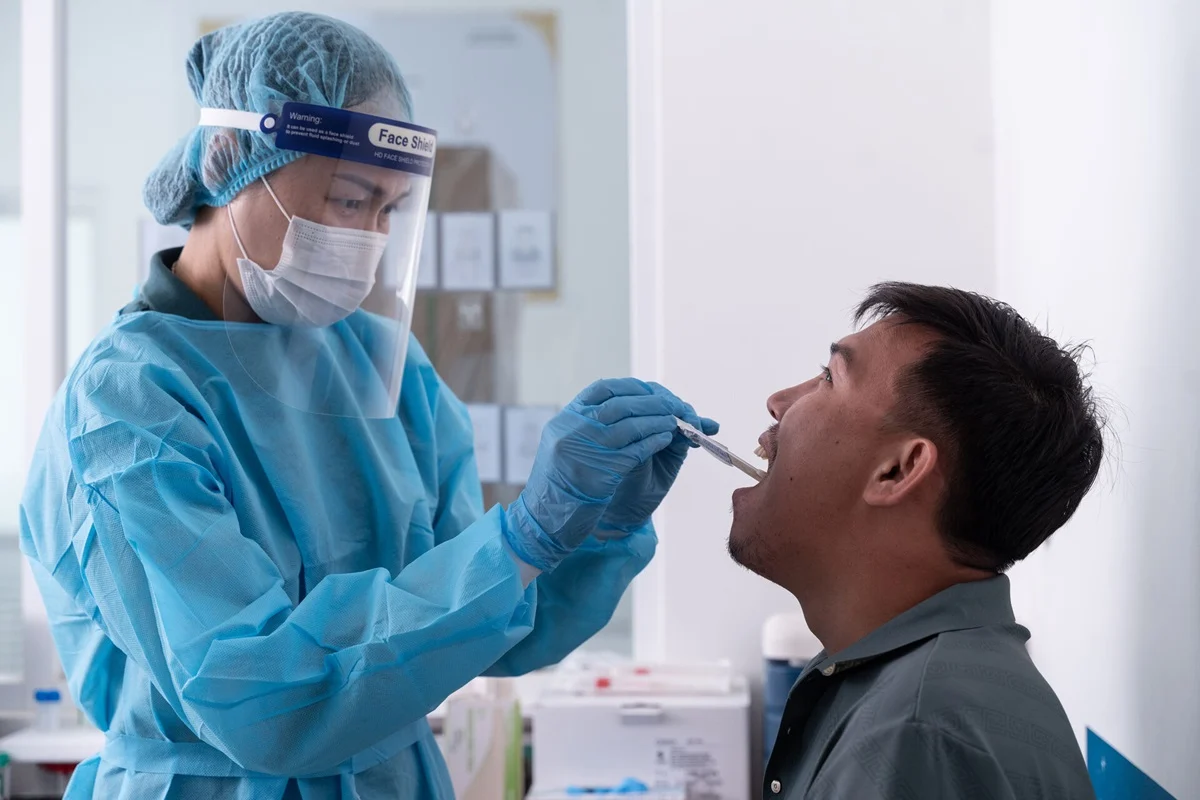
A major hurdle in TB detection has always been the difficulty some patients face in providing a sputum sample. Children, adolescents, and people living with HIV often struggle to produce the deep-lung mucus required for traditional testing. To address this, the WHO now recommends the use of tongue swabs. This non-invasive method involves simply swabbing the surface of the tongue to collect DNA from the TB bacteria. This breakthrough is expected to significantly increase detection rates among pediatric populations and those with paucibacillary TB, where bacterial loads are lower.
In addition to tongue swabs, the WHO has endorsed a cost-saving strategy known as sputum pooling. This method involves combining samples from multiple individuals into a single test run. If the pool tests negative, all individuals in that group are cleared. If the pool tests positive, individual samples are then tested to identify the infected person. This approach is particularly effective in high-burden, resource-constrained settings, as it maximizes the utility of expensive reagents and reduces the time machines spend processing samples. Research suggests that pooling can increase testing capacity by up to 400% in certain scenarios, providing a vital lifeline for programs operating under tight budget constraints.
A Chronology of the Global Fight Against Tuberculosis
To understand the urgency of the 2026 call to action, it is necessary to view the current efforts within the context of a decades-long struggle. Tuberculosis was identified by Robert Koch in 1882, yet it remains a leading infectious killer more than 140 years later. The modern era of TB control began in earnest in the late 1990s with the DOTS (Directly Observed Treatment, Short-course) strategy, which evolved into the "End TB Strategy" adopted by the World Health Assembly in 2014.
Since the turn of the millennium, global efforts have saved an estimated 83 million lives. However, the progress has been uneven. The COVID-19 pandemic caused significant disruptions, reversing years of gains as resources were diverted and lockdowns prevented patients from accessing care. In 2023, the United Nations High-Level Meeting on TB saw world leaders commit to ambitious targets, including reaching 90% of people with TB prevention and care services by 2027. The 2026 World TB Day serves as a critical milestone on the road to those 2027 targets, acting as a progress report and a catalyst for the final push toward the 2030 Sustainable Development Goals.
The Human and Economic Toll of TB
Despite being preventable and curable, tuberculosis continues to exert a devastating toll on global society. Current data indicates that approximately 3,300 people die from TB every day, amounting to over 1.2 million deaths annually. Furthermore, 29,000 people fall ill with the disease daily. These figures are not merely health statistics; they represent a massive economic burden. TB primarily affects adults in their most productive years, leading to lost wages, decreased productivity, and increased poverty for families.
The WHO highlights that investing in TB control is not just a moral imperative but a strategic economic choice. For every US dollar invested in TB prevention and treatment, there is a projected return of up to $43 in health and economic benefits. This high return on investment (ROI) stems from the restoration of the workforce and the prevention of catastrophic health expenditures that often push families into extreme poverty. Dr. Tereza Kasaeva, Director of WHO’s Department for HIV, Tuberculosis, Hepatitis and Sexually Transmitted Infections, emphasized that decisive leadership and strategic investment are the only ways to unlock these economic returns and protect global health security.
Integrating Services: The One-Stop-Shop Model
One of the most innovative aspects of the new diagnostic devices is their versatility. While primarily used for TB, many of these molecular platforms can be configured to test for other infectious diseases, including HIV, mpox, and Human Papillomavirus (HPV). This capability supports the "one-stop-shop" service model, where a patient can be screened for multiple conditions during a single visit.
This integrated approach is particularly beneficial for people living with HIV, who are significantly more likely to develop active TB. By utilizing point-of-care urine tests for TB in HIV-positive patients alongside molecular diagnostics, health systems can provide a comprehensive care package that addresses co-morbidities simultaneously. This patient-centered approach improves equity in healthcare delivery and ensures that diagnostic infrastructure is used to its maximum potential, creating a more resilient health system capable of responding to both existing and emerging infectious threats.
Addressing the Funding Crisis and Research Gaps
Despite the clear benefits of ending TB, the global response is currently hampered by a severe lack of funding. Global health funding for TB has seen significant cuts in recent years, threatening to undo decades of progress. The WHO estimates that there is an annual shortfall of approximately $5 billion for TB research and development alone. This funding gap slows the development of new medicines, more effective diagnostics, and, most importantly, a new vaccine.
The only currently available vaccine, BCG, was developed over a century ago. While it provides some protection for infants against severe forms of TB, its effectiveness in preventing pulmonary TB in adults is limited. To bridge this gap, the WHO has launched the TB Vaccine Accelerator Council. This initiative aims to align governments, funders, and the private sector to fast-track the development of new vaccine candidates. Several promising vaccines are currently in late-stage clinical trials, but without sustained financial commitment, their journey from the lab to the clinic could be delayed by years.
Implications for Global Health Security
The fight against TB is also a fight against antimicrobial resistance (AMR). Rifampicin-resistant TB (RR-TB) and multi-drug-resistant TB (MDR-TB) are major components of the global AMR crisis. When TB is not diagnosed promptly or when treatment is interrupted, the bacteria can develop resistance to standard drugs, making the disease much harder and more expensive to treat. The new WHO guidelines on rapid diagnostics are a critical tool in this battle, as they allow for the early detection of drug resistance, ensuring that patients are placed on the correct treatment regimen from the outset.
The WHO’s 2026 call to action serves as a reminder that TB is a central pillar of health security. An uncontrolled TB epidemic fuels the development of drug-resistant pathogens that can cross borders with ease. Therefore, achieving universal health coverage and ending the TB epidemic are inextricably linked. The organization urges all member states to prioritize TB within their national health budgets and to treat the disease as a priority for both domestic and international security.
Conclusion: The Path Forward to 2030
As the global community reflects on the progress made by World TB Day 2026, the message from the WHO is clear: the tools to end tuberculosis exist, but the political will and financial resources must catch up to the science. The transition to near-point-of-care testing, the adoption of non-invasive sampling like tongue swabs, and the implementation of efficient strategies like sputum pooling offer a roadmap to reaching the millions who are currently missed by health systems.
The success of these initiatives depends on a multi-sectoral approach that involves not just health ministries, but also finance, labor, and social development sectors. By focusing on country-led initiatives and empowering communities to take charge of their own health, the goal of ending TB by 2030 remains a viable possibility. The WHO continues to stand with partners and survivors to advocate for a world where no one dies from a disease that is both preventable and curable. The innovations highlighted today are the keys to that future, representing a critical step toward health equity and a world free of tuberculosis.