The World Health Organization (WHO) has issued a high-level call to action on World TB Day 2026, urging the international community to dismantle the barriers preventing the total eradication of tuberculosis. Central to this year’s mission is the rapid deployment of groundbreaking diagnostic innovations, including point-of-care molecular tests and non-invasive tongue swabs, which promise to bring high-quality healthcare directly to the most vulnerable populations. As tuberculosis (TB) remains one of the world’s most lethal infectious diseases, the WHO’s updated guidelines represent a strategic shift toward decentralized, patient-centered care. By moving diagnosis out of distant, centralized laboratories and into local clinics or community settings, health officials aim to close the "diagnostic gap" that leaves millions of cases undetected every year.
Revolutionizing Detection with Point-of-Care Innovations
For decades, the diagnosis of tuberculosis has relied heavily on centralized laboratory infrastructure, often requiring patients to travel long distances or wait days for results. The new WHO guidelines focus on portable, battery-powered diagnostic tools that can be operated by minimally trained health workers in remote areas. These devices deliver results in less than sixty minutes, a fraction of the time required by traditional methods. Furthermore, these new tools are available at less than half the cost of many existing molecular diagnostics, making them a financially viable option for low- and middle-income countries struggling with high disease burdens.
The impact of this shift cannot be overstated. When a patient can be tested and diagnosed during a single visit, the likelihood of "loss to follow-up"—where a patient never returns to receive their results or start treatment—is drastically reduced. Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, emphasized that these tools are transformative. According to Dr. Tedros, bringing fast and accurate diagnosis closer to the people not only saves individual lives but also curbs the transmission of the bacteria within communities, ultimately reducing the long-term economic burden on national health systems.
New Sample Collection Methods: The Rise of Tongue Swabs
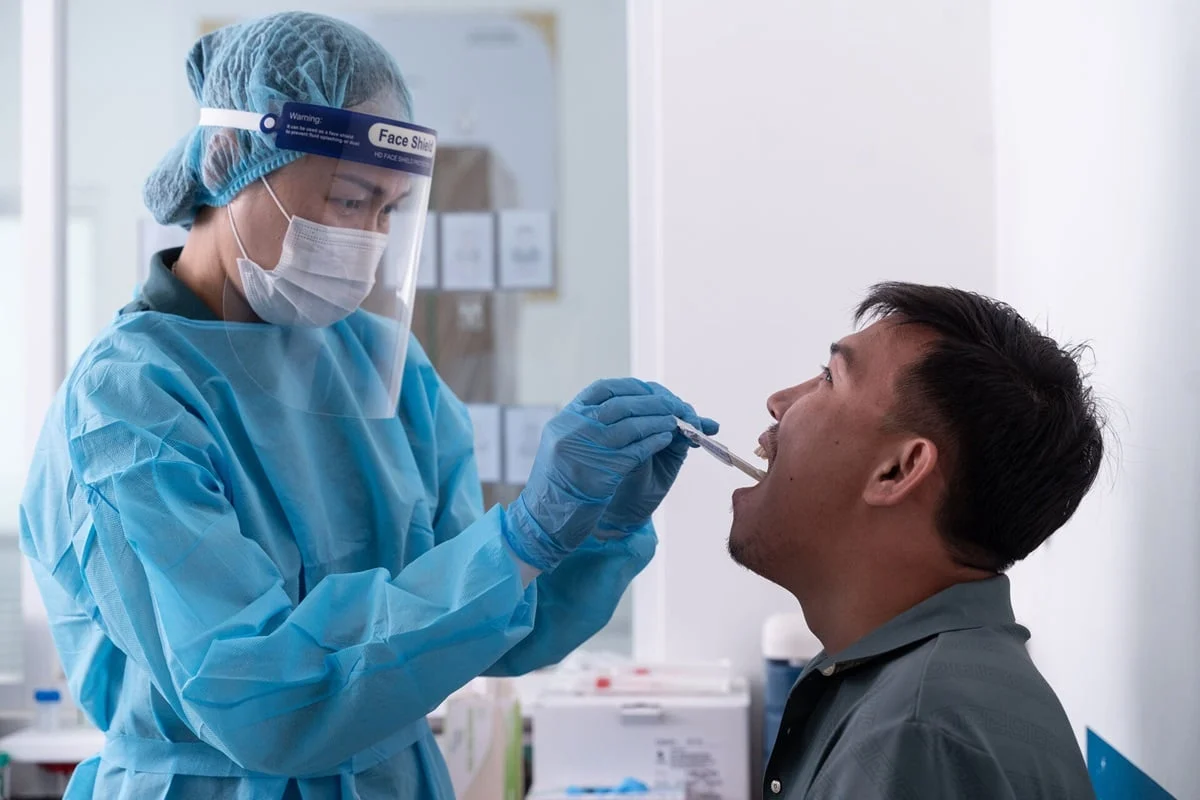
One of the most significant hurdles in TB diagnosis has historically been the collection of sputum—the thick phlegm coughed up from the lungs. Many patients, particularly children, adolescents, and those living with HIV, find it difficult or impossible to produce an adequate sputum sample. This has led to underdiagnosis and higher mortality rates among these specific groups. To address this, the WHO now recommends the use of tongue swabs as a primary sample collection method.
Tongue swabs are simple to administer, non-invasive, and do not require the patient to perform the forceful coughing necessary for sputum collection. This innovation is expected to significantly increase the detection of TB in pediatric populations and among those with advanced HIV, who are at the highest risk of rapid disease progression. By expanding the "diagnostic toolkit" to include these easier methods, the WHO is ensuring that no patient is left behind simply because they could not provide a traditional sample.
In tandem with tongue swabs, the WHO is advocating for a "sputum pooling" strategy. This approach involves combining samples from multiple individuals and testing them in a single batch. If the pool tests negative, all individuals in that group are cleared. If the pool tests positive, the individual samples are then tested separately. This method is a critical resource-management tool, particularly in settings where diagnostic machines or chemical reagents are in short supply. Sputum pooling maximizes the efficiency of existing laboratory equipment and significantly lowers the cost per person tested.
The Global Burden: Analyzing the Current Crisis
Despite being a preventable and curable disease, tuberculosis continues to exert a devastating toll on global health. Current data indicates that more than 3,300 people die from TB every single day, amounting to over 1.2 million deaths annually. Furthermore, approximately 29,000 people fall ill with the disease every 24 hours. While global efforts have saved an estimated 83 million lives since the turn of the millennium, the progress is fragile.
The WHO reports that the uptake of rapid diagnostic tools has been sluggish in many regions. This delay is attributed to high initial procurement costs, a lack of consistent electricity in rural clinics, and a historical reliance on sample transport networks that are often unreliable. The introduction of battery-powered, low-cost molecular tests is designed specifically to bypass these infrastructural hurdles. By integrating these tools into the primary healthcare level, countries can move toward the global target of universal access to drug-susceptibility testing, ensuring that patients are not only diagnosed with TB but also screened for rifampicin-resistance, a form of the disease that is much harder to treat.
Economic Implications and the Funding Gap
The fight against tuberculosis is as much an economic challenge as it is a medical one. Dr. Tereza Kasaeva, Director of the WHO’s Department for HIV, Tuberculosis, Hepatitis, and Sexually Transmitted Infections, pointed out that investing in TB eradication is a strategic economic choice. For every US dollar invested in TB prevention and treatment, there is a projected return of up to $43 in health and economic benefits. This return manifests through increased labor productivity, reduced healthcare spending, and the prevention of the catastrophic household costs that often plunge families into poverty when a breadwinner falls ill with TB.
However, the global funding landscape remains bleak. There is an estimated annual gap of $5 billion in funding for TB research and development. This shortfall hampers the creation of new medicines, more effective diagnostics, and, most importantly, a new vaccine. The current BCG vaccine, while effective in preventing severe forms of TB in children, offers limited protection for adults against the pulmonary form of the disease, which is responsible for most transmissions. To bridge this gap, the WHO has spearheaded the TB Vaccine Accelerator Council, an initiative aimed at aligning governments, private funders, and the pharmaceutical industry to fast-track the development of next-generation vaccines.
World TB Day 2026: A Vision for People-Powered Progress
The theme for World TB Day 2026, “Yes! We can end TB: Led by countries, powered by people,” reflects a shift in strategy toward community-led interventions. The WHO is calling on governments to treat TB not as a siloed medical issue, but as a central pillar of national health security and Universal Health Coverage (UHC).
The 2026 roadmap emphasizes three critical pillars:
- Political Leadership: Ensuring that national leaders prioritize TB in their budgets and health policies.
- Strategic Investment: Closing the $5 billion research gap and subsidizing the rollout of point-of-care diagnostics.
- Community Empowerment: Involving TB survivors and community health workers in the design and delivery of services to reduce stigma and improve treatment adherence.
Beyond the immediate scope of tuberculosis, the WHO notes that the diagnostic infrastructure being built for TB has "multi-pathogen" potential. The same portable devices used for TB can often be adapted to test for HIV viral load, mpox, and Human Papillomavirus (HPV). This "one-stop-shop" service model makes the healthcare system more equitable and patient-centered, allowing individuals to be screened for multiple conditions during a single clinic visit.
Chronology of Progress and Future Outlook
The journey toward TB elimination has seen significant milestones, but also major setbacks. From 2000 to 2019, the world saw a steady decline in TB incidence and mortality. However, the COVID-19 pandemic caused a massive disruption in TB services, as diagnostic machines and personnel were diverted to the viral response. 2021 and 2022 marked the first time in over a decade that TB deaths increased globally.
By 2024 and 2025, the global health community began to regain lost ground, largely through the aggressive adoption of digital health tools and expanded screening programs. The 2026 guidelines represent the "third wave" of this recovery, focusing on the decentralization of technology. The goal is to meet the United Nations Sustainable Development Goal (SDG) of ending the TB epidemic by 2030.
As the world marks World TB Day 2026, the message from the WHO is clear: the tools to end tuberculosis exist, but the will to fund and implement them at scale remains the final hurdle. The transition from laboratory-based testing to point-of-care diagnostics, the move from sputum to tongue swabs, and the shift from top-down mandates to community-led care are the essential components of a strategy that could finally relegate tuberculosis to the history books. Success will require decisive leadership and a recognition that health security is a global responsibility, where an infection in one corner of the world remains a threat to all.