The World Health Organization has issued an urgent call to the international community to accelerate the implementation of new diagnostic technologies and increase strategic investment to end the global tuberculosis epidemic. Marking World TB Day 2026 under the theme "Yes! We can end TB: Led by countries, powered by people," the health body emphasized that while significant strides have been made in saving lives over the past two decades, the pace of progress remains insufficient to meet global targets. Central to this renewed push is the introduction of groundbreaking diagnostic guidelines that utilize point-of-care testing and non-invasive sample collection methods, such as tongue swabs, to reach underserved populations who have historically been excluded from traditional screening processes.
A Paradigm Shift in Tuberculosis Diagnosis
The cornerstone of the WHO’s 2026 strategy is the decentralization of diagnostic services. For decades, tuberculosis (TB) detection relied heavily on centralized laboratory infrastructure and the collection of sputum—a thick mucus coughed up from the lower airways. This process often posed significant barriers, as many patients, particularly children and individuals living with HIV, struggle to produce adequate sputum samples. Furthermore, the requirement for sophisticated laboratory equipment meant that patients in rural or resource-constrained settings often faced long wait times for results, leading to delays in treatment and continued community transmission.
The new WHO guidelines introduce portable, battery-operated diagnostic tests that can be deployed at the primary healthcare level. These devices are designed to operate in challenging environments, delivering highly accurate molecular results in less than an hour. By bringing the laboratory to the patient, these innovations eliminate the need for complex sample transport systems and reduce the cost of diagnosis to less than half of previous molecular methods.
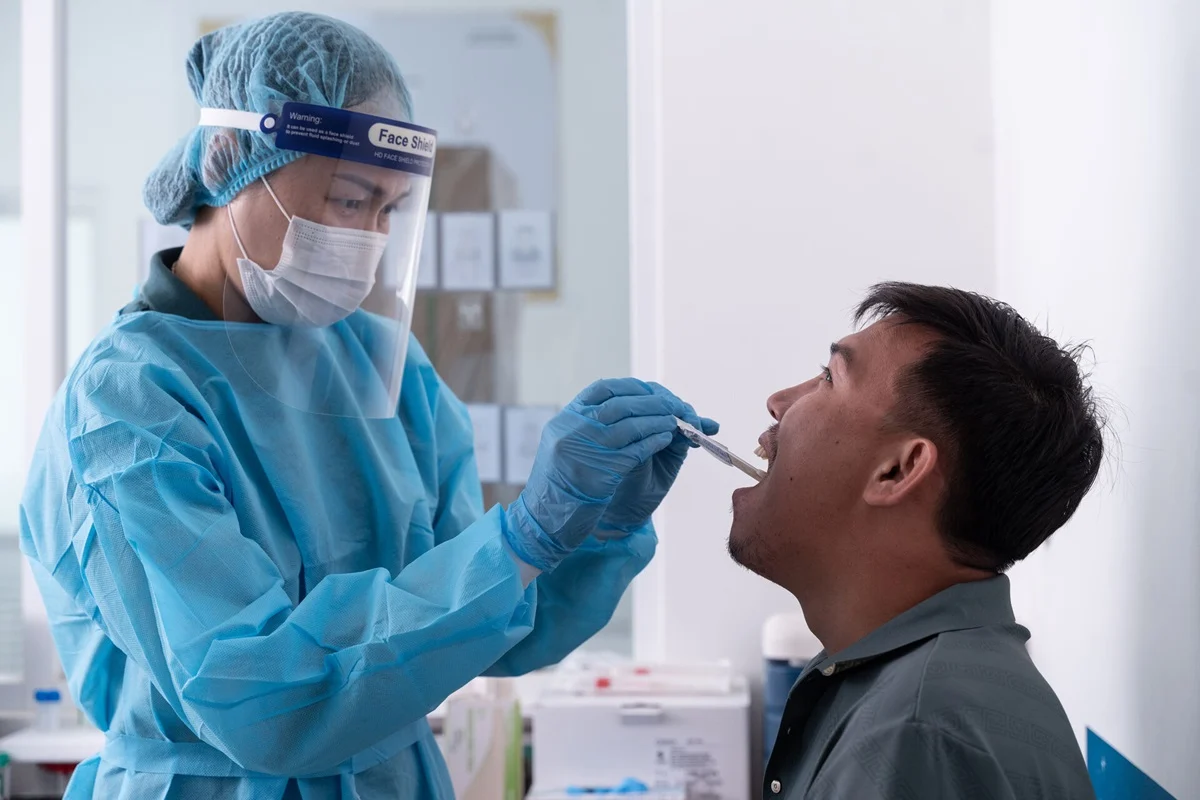
Supplementing these hardware innovations are new sample collection protocols. The WHO now officially recommends the use of tongue swabs, a simple and painless method that allows for the detection of TB DNA in the mouth. This development is particularly transformative for adolescents and adults who cannot produce sputum, ensuring that those at the highest risk of mortality are no longer overlooked. Additionally, the guidelines endorse "sputum pooling"—a process where samples from multiple individuals are tested simultaneously. If a pool tests negative, all individuals in that group are cleared; if positive, individual samples are then tested. This strategy significantly reduces the consumption of expensive reagents and maximizes the efficiency of diagnostic machinery in high-burden, low-resource settings.
The Economic and Human Cost of Inaction
Tuberculosis remains a premier global health threat, claiming more than 3,300 lives every day. According to the latest WHO data, approximately 29,000 people fall ill with the disease daily, despite it being both preventable and curable. While global efforts have saved an estimated 83 million lives since the turn of the millennium, the progress is currently categorized as "fragile."
Dr. Tedros Adhanom Ghebreyesus, WHO Director-General, highlighted the transformative potential of the new tools but warned that technology alone is not a silver bullet. "These new tools could be truly transformative for tuberculosis by bringing fast, accurate diagnosis closer to people, saving lives, curbing transmission, and reducing costs," Dr. Tedros stated. However, he underscored that the effectiveness of these innovations depends entirely on the willingness of nations to scale up access and integrate them into their national health systems.
The economic argument for ending TB is as compelling as the moral one. Dr. Tereza Kasaeva, Director of the WHO’s Department for HIV, Tuberculosis, Hepatitis, and Sexually Transmitted Infections, noted that investing in TB programs yields one of the highest returns in public health. For every US$1 invested in TB prevention and treatment, there is an estimated return of up to US$43 in health and economic gains. This return stems from increased workforce productivity, reduced healthcare expenditures on advanced disease stages, and the prevention of orphanhood and family poverty often caused by the death of a primary breadwinner.
Chronology of the Global Fight Against Tuberculosis
The 2026 World TB Day milestones are part of a long-standing international effort to eradicate a disease that has plagued humanity for millennia. To understand the current urgency, it is essential to view the timeline of modern interventions:
- 1882: Dr. Robert Koch announces the discovery of Mycobacterium tuberculosis, the bacterium that causes TB, providing the first step toward diagnosis and treatment.
- 1993: The WHO declares TB a global health emergency as cases surge alongside the HIV/AIDS epidemic.
- 2000: The Millennium Development Goals (MDGs) are established, aiming to halt and begin reversing the incidence of TB by 2015.
- 2014: The World Health Assembly approves the "End TB Strategy," which targets a 95% reduction in TB deaths and a 90% reduction in incidence by 2035.
- 2018: The first-ever UN High-Level Meeting on TB results in a political declaration to reach 40 million people with care by 2022.
- 2023: The second UN High-Level Meeting reaffirms global commitments, specifically focusing on the development of a new TB vaccine within five years.
- 2026: The WHO launches the current push for point-of-care diagnostics and non-invasive testing to close the "detection gap," where millions of cases go undiagnosed annually.
Bridging the Funding Gap and Fostering Innovation
Despite the clear economic benefits, global funding for TB remains severely depleted. The WHO estimates that there is an annual funding gap of approximately US$5 billion for research and development alone. This shortfall has slowed the development of new medicines, shorter treatment regimens, and, most critically, a highly effective vaccine.
Currently, the BCG vaccine, which is over a century old, remains the only licensed vaccine for TB. While it provides some protection for infants against severe forms of the disease, it is largely ineffective in preventing pulmonary TB in adolescents and adults, who are the primary drivers of transmission. To address this, the WHO has championed the TB Vaccine Accelerator Council. This initiative aims to align the interests of governments, philanthropic organizations, and the private sector to fast-track the clinical trial process and ensure that once a vaccine is developed, it is distributed equitably across the globe.
The diagnostic devices being championed in 2026 are also designed with "multi-pathogen" capabilities. The WHO envisions a "one-stop-shop" healthcare model where the same portable machine used to test for TB can also screen for HIV, mpox, and Human Papillomavirus (HPV). This integrated approach not only maximizes the utility of the hardware but also provides a more patient-centered experience, allowing individuals to be screened for multiple conditions during a single clinic visit.
Regional Challenges and the Path to Universal Health Coverage
The burden of tuberculosis is not distributed evenly across the globe. The majority of cases occur in the WHO South-East Asia Region, the African Region, and the Western Pacific Region. Countries such as India, Indonesia, China, the Philippines, and Pakistan often account for a significant percentage of the global caseload. In these regions, the challenges are multifaceted, involving not just medical hurdles but also social determinants of health such as malnutrition, poor housing, and the stigma associated with the disease.
The WHO’s 2026 directive emphasizes that TB must be a central pillar of the broader Universal Health Coverage (UHC) and health security agendas. The COVID-19 pandemic demonstrated how quickly infectious diseases can disrupt global stability, and TB, as a leading infectious killer, poses a constant threat to that stability. By strengthening TB diagnostic networks, countries are essentially building the infrastructure needed to respond to future respiratory pandemics.
Furthermore, the rise of Rifampicin-resistant TB (RR-TB) and Multi-drug-resistant TB (MDR-TB) adds a layer of complexity to the crisis. These forms of the disease require longer, more expensive, and more toxic treatment regimens. The new near-point-of-care tests are capable of detecting drug resistance almost immediately, allowing clinicians to put patients on the correct treatment path from day one, thereby preventing the further spread of resistant strains.
Analysis of Global Implications
The shift toward point-of-care diagnostics and tongue swab testing represents more than just a technological upgrade; it is a shift in the philosophy of public health. By prioritizing ease of use and accessibility, the WHO is attempting to democratize healthcare. If successfully scaled, these tools will significantly reduce the "missing millions"—the estimated one-third of people with TB who are not reached by health systems each year.
However, analysts point out that the success of the 2026 initiative hinges on political will. While the WHO provides the technical guidelines and the evidence base, the actual procurement and deployment of these tools depend on national budgets and international aid. The reduction in global health funding seen in the wake of the pandemic remains a significant hurdle. If the US$5 billion research gap is not closed, the world may miss the opportunity to deploy a new vaccine by the end of the decade, potentially extending the epidemic for several more generations.
As World TB Day 2026 concludes, the message from the World Health Organization is clear: the tools to end tuberculosis are within reach, but they require a level of investment and political courage that matches the scale of the crisis. The transition from laboratory-based testing to community-based diagnosis marks the beginning of a new chapter in the fight against TB—one where the focus is on reaching the most vulnerable, wherever they may be. Through decisive leadership and the rapid implementation of these innovations, the WHO maintains that the goal of a TB-free world remains an achievable reality.