Major depressive disorder (MDD) stands as a pervasive and debilitating global health crisis, claiming its place as a leading cause of disability worldwide. Despite the availability of numerous antidepressant medications, a significant proportion of individuals—approximately 30%—experience treatment-resistant depression (TRD). This means their symptoms fail to respond adequately to conventional pharmacological interventions, leaving them in a state of persistent suffering. In recent years, ketamine has emerged as a beacon of hope for this vulnerable population, demonstrating remarkable rapid-acting antidepressant effects. However, the precise molecular pathways through which ketamine exerts its influence within the intricate circuitry of the human brain have remained largely elusive. This lack of understanding has presented a substantial hurdle in optimizing and personalizing ketamine-based therapies.
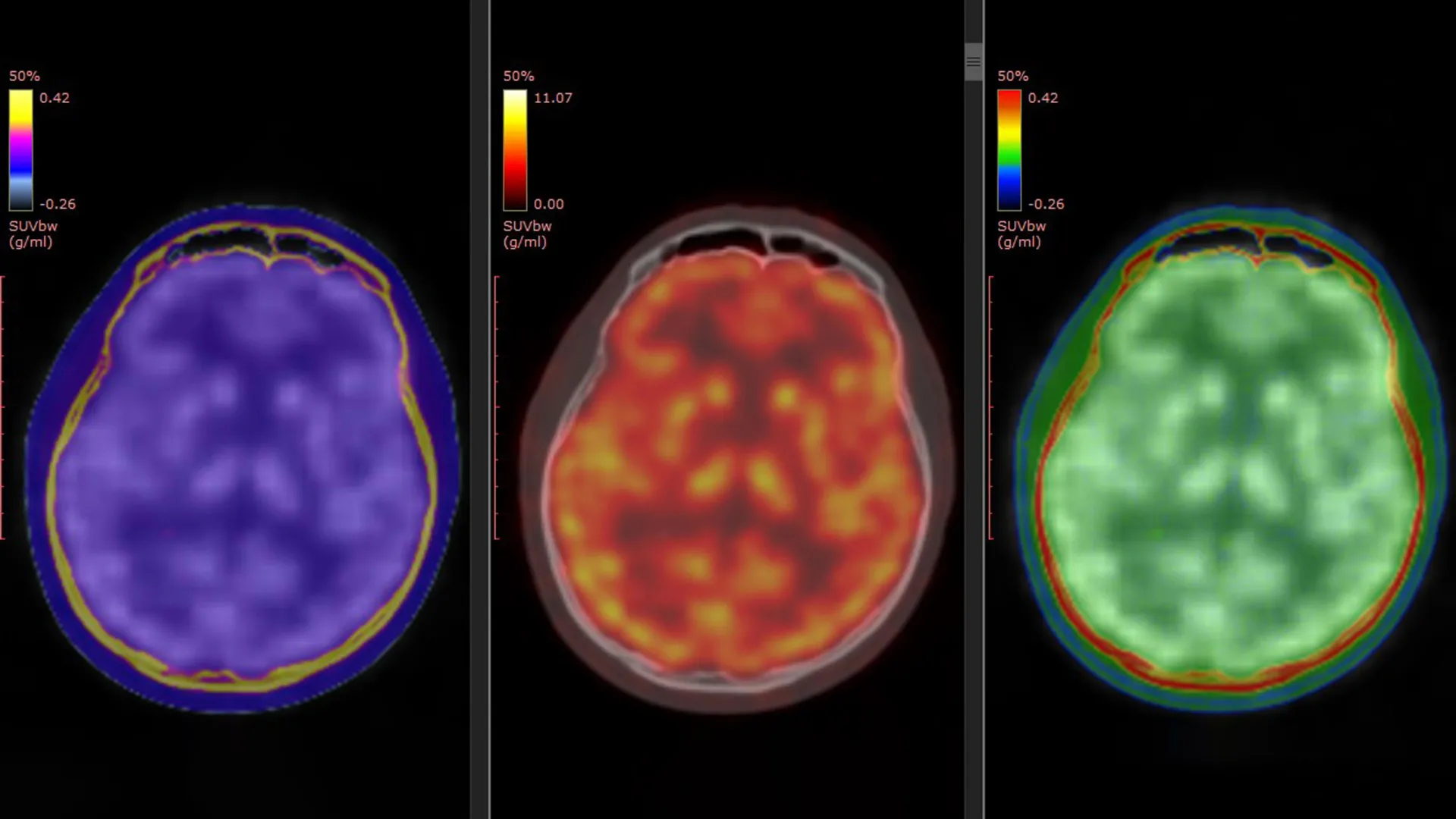
A groundbreaking study, published on March 5, 2026, in the esteemed journal Molecular Psychiatry, has significantly advanced our comprehension of this complex pharmacological puzzle. Spearheaded by Professor Takuya Takahashi of the Department of Physiology at Yokohama City University Graduate School of Medicine in Japan, the research team employed a cutting-edge positron emission tomography (PET) imaging technique to directly visualize alterations in glutamate $alpha$-amino-3-hydroxy-5-methyl-4-isoxazole propionic acid receptors (AMPARs). These receptors are critical protein components that govern neuronal communication and play a pivotal role in synaptic plasticity and glutamatergic signaling—processes that are profoundly affected in patients undergoing ketamine treatment.
Professor Takahashi articulated the significance of their findings, stating, "Although ketamine has shown rapid antidepressant effects in patients with treatment-resistant depression, its molecular mechanism in the human brain has remained unclear. Our research provides the first direct evidence in humans, visualizing how ketamine impacts AMPARs in specific brain regions and links these changes to symptom relief."
Visualizing Brain Receptors with a Novel PET Tracer
The cornerstone of this pioneering research was the utilization of a novel PET tracer, designated as [11C]K-2, developed by Professor Takahashi’s team. This sophisticated tracer possesses the unique capability to visualize cell-surface AMPARs directly within the living human brain. Prior experimental and preclinical studies had strongly suggested a role for AMPAR activity in mediating ketamine’s antidepressant effects. This new investigation transcends those hypotheses by offering direct empirical validation in human subjects.
To achieve this crucial insight, the researchers meticulously compiled and analyzed data from three meticulously conducted registered clinical trials that had previously taken place in Japan. The study cohort comprised 34 individuals diagnosed with TRD and 49 healthy volunteers who served as a control group, ensuring a robust comparison framework.
Participants diagnosed with TRD were administered either intravenous ketamine or a placebo over a rigorous two-week treatment period. To capture the dynamic effects of the intervention, PET brain imaging was performed at two critical junctures: immediately preceding the commencement of treatment and again following the final ketamine or placebo infusion. This longitudinal imaging design enabled the researchers to precisely quantify and compare changes in AMPAR levels and their spatial distribution within the brain over the course of the study.
Region-Specific Brain Changes Linked to Symptom Relief
The comprehensive analysis of the PET imaging data revealed a compelling pattern of AMPAR distribution in individuals with TRD. Specifically, the study identified widespread abnormalities in AMPAR density when compared to their healthy counterparts. Crucially, these observed differences were not diffuse across the entire brain but were concentrated within distinct, anatomically defined brain regions.
Furthermore, the administration of ketamine did not elicit a uniform effect on AMPARs throughout the brain. Instead, the improvements experienced by patients in their depressive symptoms were intricately associated with dynamic, region-specific modulations of AMPAR levels. In some cortical areas, researchers observed an increase in AMPAR density, suggesting enhanced neuronal signaling. Conversely, other regions, particularly those implicated in reward processing such as the habenula, showed a reduction in AMPARs. These nuanced, localized shifts in AMPAR distribution were found to be strongly correlated with the degree of symptom amelioration experienced by the patients.
"Ketamine’s antidepressant effect in patients with TRD is mediated by dynamic changes in AMPAR in the living human brain," Professor Takahashi elaborated. "Using a novel PET tracer, [11C]K-2, we were able to visualize how ketamine alters AMPAR distribution across specific brain regions and how these changes correlate with improvements in depressive symptoms."
These findings represent a significant leap forward, providing the first direct human evidence that substantiates mechanisms previously inferred from animal studies and directly links them to tangible clinical antidepressant outcomes.
Potential Biomarker for Predicting Treatment Response
The implications of this research extend far beyond simply elucidating the neurobiological underpinnings of ketamine’s efficacy. The study’s findings hold substantial promise for immediate clinical application. The capacity to visualize AMPAR density using PET imaging could potentially be developed into a valuable biomarker. Such a biomarker could empower clinicians to more accurately assess and predict an individual’s likelihood of responding to ketamine treatment for TRD.
In the realm of mental health, the identification of reliable biological markers that can forecast treatment response remains a paramount objective, particularly given the considerable number of patients who do not benefit from standard antidepressant therapies. This research offers a tangible pathway toward achieving that goal.
Toward More Personalized Depression Treatments
By providing scientists with the unprecedented ability to directly observe AMPAR activity in the living human brain, this study effectively bridges a long-standing chasm between fundamental laboratory research and the practical realities of clinical psychiatry. The results unequivocally establish AMPAR modulation as a central mechanistic player in ketamine’s rapid antidepressant effects. Moreover, they strongly suggest that AMPAR PET imaging could serve as a crucial tool in guiding the development of more individualized and effective treatment strategies for TRD in the future.
Ultimately, this pioneering work paves the way for the creation of more precise and targeted therapeutic interventions for individuals grappling with the profound challenges of treatment-resistant depression, offering renewed hope for improved patient outcomes and enhanced quality of life. The research was made possible through the generous support of several esteemed institutions, including the Ministry of Education, Culture, Sports, Science and Technology (Special Coordination Funds for Promoting Science and Technology); the Japan Agency for Medical Research and Development (AMED) under grant numbers JP18dm0207023, JP19dm0207072, JP24wm0625304, JP25gm7010019, and JP20dm0107124; the Japan Society for the Promotion of Science KAKENHI with grant numbers 22H03001, 20H00549, 20H05922, 23K10432, 19H03587, 20K20603, 22K15793, and 21K07508; the Takeda Science Foundation; the Keio Next-Generation Research Project Program; the SENSHIN Medical Research Foundation; and the Japan Research Foundation for Clinical Pharmacology.
Context and Background: The Growing Challenge of Treatment-Resistant Depression
The global mental health landscape is continually grappling with the profound impact of depression. According to the World Health Organization (WHO), depression is one of the most common mental disorders, affecting hundreds of millions of people worldwide. While effective treatments exist for many, the subset of individuals with TRD represents a significant unmet clinical need. The economic and social burden of TRD is immense, encompassing lost productivity, increased healthcare costs, and profound personal suffering for patients and their families.
The development of ketamine as a rapid-acting antidepressant has been a significant advancement since its initial serendipitous observations in the early 2000s. Unlike traditional antidepressants, which can take weeks to exert their effects, ketamine has been shown to alleviate depressive symptoms within hours or days of administration. This rapid onset of action is particularly crucial for individuals experiencing severe depression or suicidal ideation.
However, the exact mechanisms behind ketamine’s swift therapeutic effects have been a subject of intense scientific inquiry. Early research pointed towards its action as an N-methyl-D-aspartate (NMDA) receptor antagonist, a class of drugs known for their anesthetic properties. But the antidepressant effects appeared to be dissociated from its NMDA receptor blockade, suggesting a more complex cascade of downstream events. The role of AMPA receptors, which are activated by glutamate, a primary excitatory neurotransmitter, emerged as a key area of investigation. AMPA receptors are critical for synaptic plasticity, the process by which neural connections are strengthened or weakened over time, a fundamental mechanism underlying learning and memory, and crucially, mood regulation.
Timeline of Discovery and Development
The journey leading to the findings published in Molecular Psychiatry on March 5, 2026, represents years of dedicated research and incremental scientific progress.
- Early 2000s: Observational studies begin to hint at the antidepressant potential of ketamine, initially noted for its anesthetic properties.
- Mid-2000s: Formal research begins to investigate ketamine’s rapid antidepressant effects in controlled clinical settings. Initial studies highlight its efficacy in treatment-resistant populations.
- Late 2000s – Early 2010s: Significant research efforts focus on understanding ketamine’s neurobiological mechanisms. The role of glutamate and its receptors, including NMDA and AMPA, becomes a central focus.
- Mid-2010s: Development of novel PET tracers for visualizing specific neurotransmitter receptors in the living human brain gains momentum.
- Late 2010s: Professor Takahashi’s team develops the PET tracer [11C]K-2, specifically designed for visualizing AMPARs. Preclinical studies validate its efficacy in animal models.
- Early 2020s: The team initiates human studies, combining the novel PET tracer with existing clinical trial data from TRD patients.
- March 5, 2026: Publication of the landmark study in Molecular Psychiatry, providing direct human evidence of ketamine’s impact on AMPARs and its correlation with symptom relief.
Broader Implications for Mental Health Care
The implications of this research are far-reaching and have the potential to reshape the landscape of depression treatment.
Personalized Medicine: The identification of AMPAR density as a potential biomarker could usher in an era of truly personalized medicine for TRD. Clinicians may soon be able to use PET scans to identify patients who are most likely to benefit from ketamine treatment, thereby avoiding ineffective therapies and associated costs and side effects. This could also lead to the development of companion diagnostics.
Drug Development: A deeper understanding of ketamine’s mechanism of action can inform the development of new antidepressant medications that specifically target AMPA receptor pathways. This could lead to the creation of more effective and potentially safer treatments with fewer side effects than ketamine itself, which has limitations regarding its abuse potential and side effects.
Therapeutic Strategies: The findings might also lead to the refinement of ketamine administration protocols, such as optimizing dosage, frequency, and duration of treatment based on individual AMPAR profiles. Furthermore, it could pave the way for combination therapies, where ketamine is used alongside other agents that modulate AMPA receptor activity.
Research into Other Neurological Conditions: The methodologies and insights gained from this study could be extended to investigate the role of AMPA receptors in other neurological and psychiatric disorders characterized by altered synaptic plasticity and glutamatergic signaling, such as anxiety disorders, bipolar disorder, and schizophrenia.
The meticulous work undertaken by Professor Takahashi and his team represents a significant stride in demystifying the complex neurobiology of depression and its treatment. By providing a clear, visualizable link between a critical brain receptor and the symptomatic relief offered by ketamine, this research not only advances scientific knowledge but also offers tangible hope for millions of individuals suffering from treatment-resistant depression, moving the field closer to more precise and effective therapeutic interventions.