New findings from the University of Cambridge illuminate a complex relationship between menopause and the female brain, suggesting significant alterations in brain structure alongside a heightened prevalence of anxiety, depression, and sleep disturbances. The comprehensive study, drawing on data from nearly 125,000 women, revealed a reduction in grey matter volume in key brain regions among post-menopausal women. This research, published in the esteemed journal Psychological Medicine, offers crucial insights into the multifaceted impact of this natural life transition.
Unpacking the Menopausal Transition
Menopause, a biological marker signifying the cessation of a woman’s menstrual periods, is primarily driven by a natural decline in hormone levels, particularly estrogen and progesterone. This transition typically occurs between the ages of 45 and 55 and is often accompanied by a spectrum of physical and psychological symptoms. These commonly include vasomotor symptoms like hot flushes and night sweats, mood fluctuations, vaginal dryness, and significant disruptions to sleep patterns. Beyond these well-documented symptoms, a growing body of research has also indicated potential links between menopause and changes in cognitive functions, such as memory, attention span, and language processing.
In England, Hormone Replacement Therapy (HRT) remains a widely prescribed treatment to alleviate menopausal symptoms, particularly those impacting mental well-being and sleep quality. In 2023 alone, an estimated 15% of women in England were prescribed HRT, underscoring its significant role in managing this life stage. Despite its widespread use, scientific understanding of the precise mechanisms by which menopause and HRT influence brain structure, cognitive abilities, and overall mental health has remained somewhat limited, prompting the need for more extensive investigations.
A Deep Dive into UK Biobank Data
To address these knowledge gaps, Cambridge researchers embarked on an ambitious analysis utilizing data from the UK Biobank, a massive biomedical database containing detailed genetic and health information from half a million UK residents. Their focus was on a cohort of nearly 125,000 women, meticulously categorized into three distinct groups to allow for nuanced comparisons. The first group comprised women who had not yet experienced menopause, serving as a baseline. The second group consisted of women who had gone through menopause and had never utilized HRT. The third and final group included post-menopausal women who had received HRT. This stratification was crucial for isolating the effects of menopause itself from those potentially mediated by HRT.
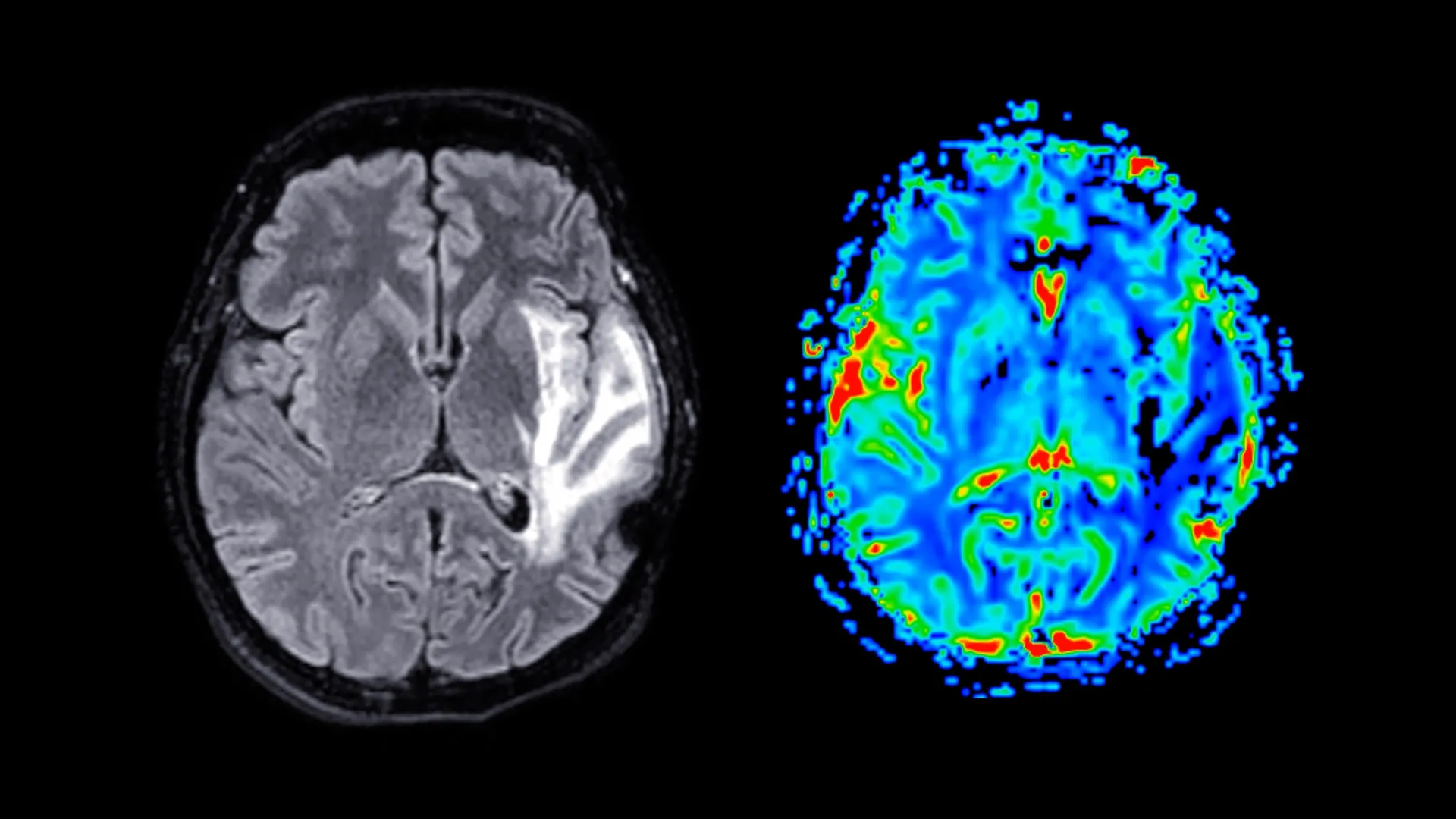
Participants in the study provided a wealth of self-reported information through comprehensive questionnaires. These surveys delved into the specifics of their menopausal symptoms, their mental health status, their sleep patterns, and their general health and well-being. Furthermore, a subset of these women underwent standardized cognitive assessments designed to evaluate key aspects of their memory and reaction times. The study also incorporated advanced neuroimaging techniques, with approximately 11,000 women participating in Magnetic Resonance Imaging (MRI) scans. These scans provided invaluable structural data of the brain, enabling researchers to identify and quantify differences in brain volume and composition.
The average age at which participants in the study reached menopause was approximately 49.5 years. For those who were prescribed HRT, the initiation of treatment typically occurred around the age of 49, suggesting that HRT was often commenced during the perimenopausal or early post-menopausal stages. This timeline is consistent with current clinical guidelines aimed at managing menopausal symptoms effectively.
Anxiety, Depression, and Sleep Disturbances Post-Menopause
The study’s findings underscore a clear association between menopause and increased psychological distress. Women who had transitioned through menopause were significantly more likely to seek medical assistance from their General Practitioner (GP) or psychiatrist for symptoms of anxiety, nervousness, or depression when compared to their pre-menopausal counterparts. This was further corroborated by higher scores on standardized depression questionnaires and a greater likelihood of having been prescribed antidepressant medications among the post-menopausal cohort.
Intriguingly, the analysis also revealed that women in the HRT group reported higher levels of anxiety and depression than those who did not use HRT. However, a deeper examination of the data suggested that these elevated levels of psychological distress were already present in these women before they began menopause or commenced HRT. This observation led the researchers to hypothesize that GPs may have been more inclined to prescribe HRT to women who already exhibited a predisposition to anxiety and depression, possibly in anticipation that menopause could exacerbate these pre-existing conditions. This highlights a complex interplay between pre-existing mental health vulnerabilities and menopausal transitions, and the clinical decision-making surrounding HRT.
Sleep disturbances emerged as another prevalent issue following menopause. Post-menopausal women were more prone to reporting symptoms of insomnia, experiencing reduced overall sleep duration, and suffering from persistent feelings of tiredness. The HRT group, while not differing significantly in total sleep duration from post-menopausal women not taking HRT, reported feeling the most fatigued of all three groups. This suggests that while HRT might not necessarily increase or decrease the quantity of sleep, it could potentially influence the subjective quality of rest and the perception of fatigue.
The Crucial Role of Lifestyle and Mental Health Support
Dr. Christelle Langley, a researcher from the Department of Psychiatry at the University of Cambridge and a key contributor to the study, emphasized the profound impact of menopause on women’s lives. "Most women will go through menopause, and it can be a life-changing event, whether they take HRT or not," Dr. Langley stated. She underscored the importance of proactive health management during this period. "A healthy lifestyle — exercising, keeping active and eating a healthy diet, for example — is particularly important during this period to help mitigate some of its effects." This advice aligns with established public health recommendations for managing chronic conditions and promoting overall well-being.
Dr. Langley also stressed the societal imperative for greater awareness and support. "We all need to be more sensitive to not only the physical, but also the mental health of women during menopause, however, and recognize when they are struggling," she urged. "There should be no embarrassment in letting others know what you’re going through and asking for help." This call for destigmatization and open communication is vital in ensuring women receive the comprehensive care they need during this significant life transition.
Cognitive Performance: Reaction Time Slows, Memory Holds Steady
The study also delved into the cognitive ramifications of menopause. Women who were post-menopausal and not using HRT exhibited a noticeable slowdown in their reaction times when compared to both pre-menopausal women and those undergoing HRT. This finding suggests a potential acceleration of age-related cognitive changes in this group. Interestingly, memory performance did not show significant differences across the three groups, indicating that while processing speed might be affected, the fundamental ability to form and recall memories remained largely intact.
Dr. Katharina Zühlsdorff, from the Department of Psychology at the University of Cambridge and a co-author of the study, provided a nuanced perspective on these cognitive changes. "As we age, our reaction times tend to get slower — it’s just a part of the natural ageing process and it happens to both women and men," she explained. "You can imagine being asked a question at a quiz — while you might still arrive at the correct answer as your younger self, younger people would no doubt get there much faster. Menopause seems to accelerate this process, but HRT appears to put the brakes on, slowing the ageing process slightly." This analogy effectively illustrates how menopause might hasten a natural age-related decline in processing speed, with HRT potentially offering a mitigating effect.
Grey Matter Reduction in Key Brain Regions
The most striking findings emerged from the brain imaging data. MRI scans revealed significant reductions in grey matter volume among post-menopausal women, irrespective of their HRT status. Grey matter, a critical component of the central nervous system, is densely packed with neuronal cell bodies. It plays a pivotal role in a vast array of cognitive functions, including information processing, motor control, memory formation, and emotional regulation.
The specific brain regions exhibiting the most pronounced grey matter reduction were particularly noteworthy. These included the hippocampus, a structure fundamental to the formation and consolidation of new memories; the entorhinal cortex, often described as the "gateway" for information flow between the hippocampus and other brain areas; and the anterior cingulate cortex, which is instrumental in managing emotions, facilitating decision-making, and directing attentional focus. The vulnerability of these specific regions is of significant concern given their known involvement in neurodegenerative diseases.
Potential Implications for Dementia Risk in Women
Professor Barbara Sahakian, the senior author of the study and a distinguished figure in the Department of Psychiatry at the University of Cambridge, offered a sobering perspective on the long-term implications of these findings. "The brain regions where we saw these differences are ones that tend to be affected by Alzheimer’s disease," Professor Sahakian stated. "Menopause could make these women vulnerable further down the line." This observation raises a critical question about the role of menopause in the increased susceptibility of women to dementia.
It is a well-established epidemiological fact that women are disproportionately affected by dementia, with nearly twice as many women as men diagnosed with the condition. Professor Sahakian suggested that the brain structural changes observed in post-menopausal women could offer a partial explanation for this disparity. "While not the whole story, it may help explain why we see almost twice as many cases of dementia in women than in men," she concluded. This research opens new avenues for understanding the biological underpinnings of sex-based differences in dementia risk and may inform future preventative strategies and therapeutic interventions.
The study’s findings underscore the need for a holistic approach to women’s health during midlife and beyond, integrating physical, mental, and neurological well-being. Further research is anticipated to explore the precise mechanisms by which hormonal changes influence brain structure and function, and to investigate potential interventions that could mitigate these effects and safeguard cognitive health throughout a woman’s life. The comprehensive nature of this Cambridge study provides a robust foundation for future investigations into the complex and often underappreciated impact of menopause on the female brain.